Year: 2017, Volume: 30, Issue: 4, July-August
Original Article
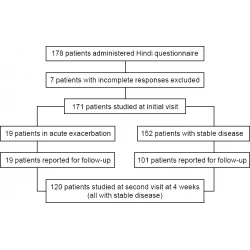
Ashutosh N Aggarwal, Isak Lallawmkima, Debasish Basu
Short Report
Ayush Lohiya, Shashi Kant, Arti Kapil, Sanjeev Kumar Gupta, Puneet Misra, Sanjay K Rai
Clinical Case Report
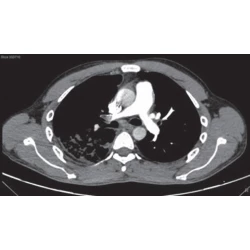
Sameer Bansal, Ketaki Utpat, Jyotsna M Joshi
Review Article
Yoon-Sook Kim, Jae-Min Park, Yeon-Sil Moon, Seol-Heui Han
Selected Summaries
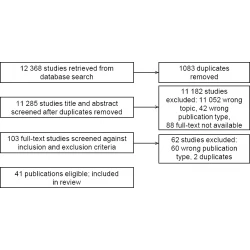
G Angeline Grace, D Bella Devaleenal
Medical Education
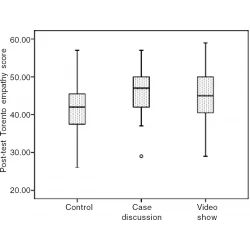
Tatjana M Ille, Ramprasad Muthukrishnan, Mihailo E Ille
Medical Education
Suman P Singh, Chirag M Modi, Chirag P Patel, Ajay G Pathak
Medicine and Society
Anju Dhawan, Raman Deep Pattanayak, Anita Chopra, VK Tikoo, Rajesh Kumar
History of Medicine
Shirish N Kavadi
Letter from Glasgow
HS Kohli
Letter from Chennai
MK Mani
Book Review
Sunil Pandya
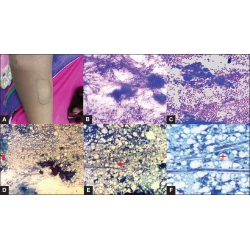
Images In Medicine
T Santosh, Hemlata Panwar, Amit Bugalia, Vandita Yogendra Singh, Nighat Hussain
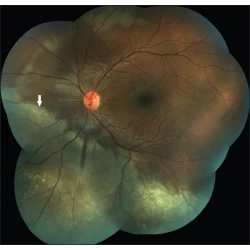
Images In Medicine
Koushik Tripathy, Rohan Chawla