Translate this page into:
Bilateral golden ring in the eye: Weill–Marchesani syndrome
A 30-year-old woman presented with decreased visual acuity in both eyes (BE) for 1 month. Her best-corrected visual acuity was 6/12 with –10 Dsph in the right eye (RE) and 6/9 with –12 Dsph in the left eye (LE). Intraocular pressure was 22 mmHg in the RE and 24 mmHg in the LE. Ocular examination revealed a small globular lens, microspherophakia with stretched zonules, causing anterior subluxation (Fig. 1). Gonioscopy revealed occludable angles in BE. Fundus examination showed advanced glaucomatous cupping in BE. Systemic examination revealed short stature, brachycephaly, short broad fingers and joint stiffness (Fig. 2). The patient was diagnosed to have Weill–Marchesani syndrome with secondary angle-closure glaucoma. She underwent Nd:YAG laser peripheral iridotomy BE and was started on ocular hypotensive medications. The patient was planned for sequential pars plana lensectomy and scleral fixated intraocular lens.
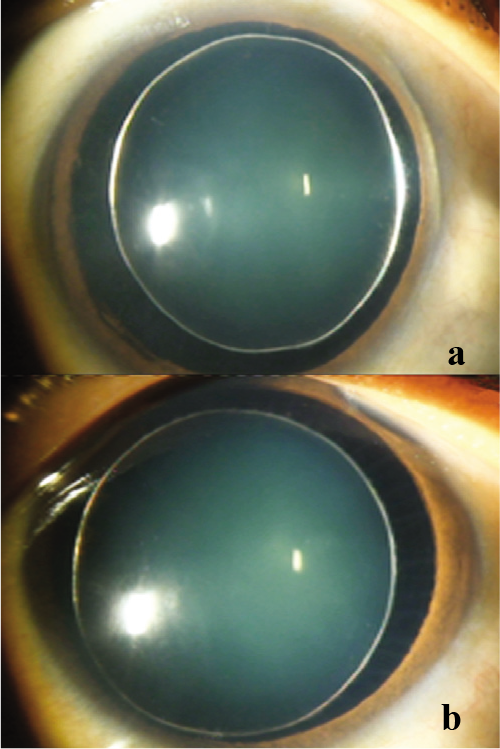
- (a and b) Slit-lamp photograph of both eyes showing small-sized spherophakic lens and golden ring due to reflection of light from 360° periphery of small crystalline globular lens with stretched zonules causing anterior subluxation in the left eye
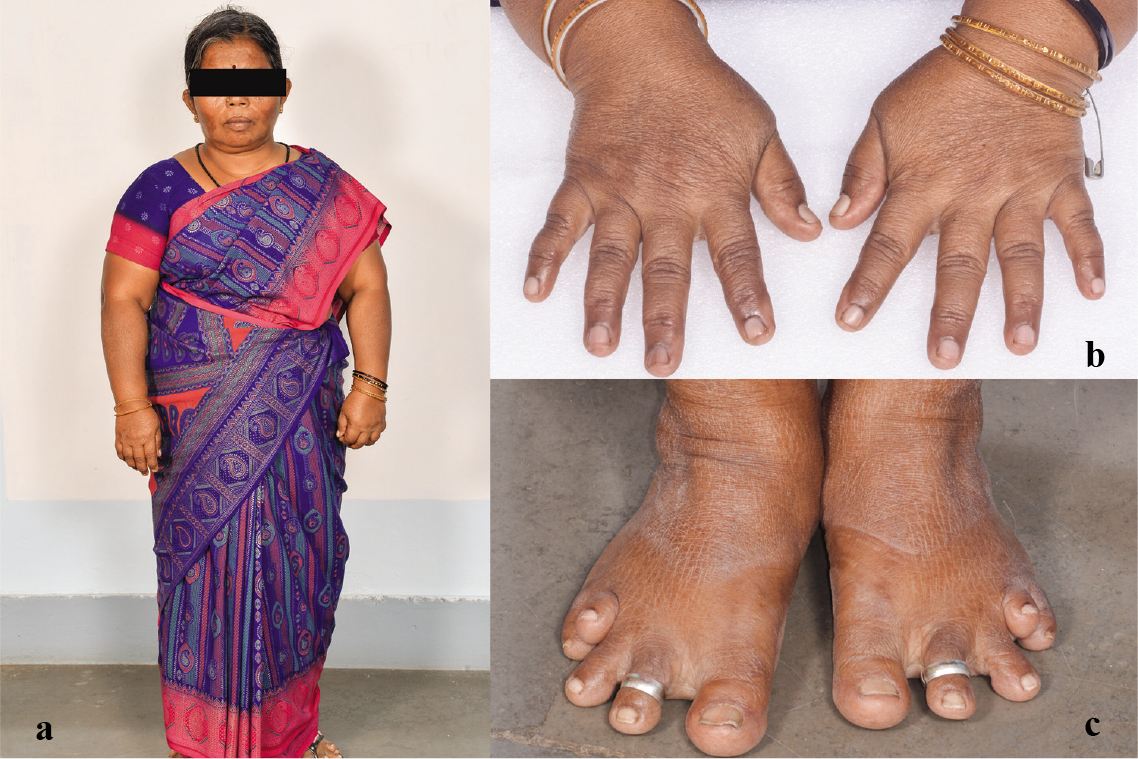
- (a–c) Clinical photograph of the patient showing short stature, short fingers and toes (brachydactyly) with deformed fourth and fifth toes
Weill–Marchesani syndrome is a multisystem disease that affects the skin, bones and joints, the heart and the eyes. Hence, cardiac evaluation should be performed before any surgical intervention. Mutations in the ADAMTS10 and FBN1 genes cause this syndrome. Early lens aspiration should be carried out in these patients when they have symptoms of decreased vision due to myopic shift as a consequence of the globular shape of the lens, otherwise pupillary block and angle-closure glaucoma develop, leading to irreversible loss of vision. Glaucoma filtration surgery or glaucoma drainage device may be required to control intraocular pressure in these patients with refractory glaucoma.
Conflicts of interest
None declared




