Translate this page into:
Hamman syndrome
2 Department of Radiodiagnosis, Military Hospital, Chennai, Tamil Nadu, India
3 Department of Medicine and Oncology, Command Hospital, Bengaluru, Karnataka, India
Corresponding Author:
J Sankar
Department of Medicine, Military Hospital, Chennai, Tamil Nadu
India
sankarjayaprakash@gmail.com
| How to cite this article: Sankar J, Uniyal M, Kumar K. Hamman syndrome. Natl Med J India 2020;33:180 |
A 19-year-old male, without any previous comorbid conditions, presented to the emergency department with a history of swelling in the neck, hoarseness of voice and fever for 1 day. Clinically, he had tachycardia, and there was crepitation in the neck and anterior chest wall on palpation. His past medical history was non-contributory, and he was not on any medication. He denied any history of trauma, surgery or any medical procedure. On chest X-ray posteroanterior view, subcutaneous emphysema was confirmed. Non-contrast computed tomography of the chest showed mediastinal and subcutaneous emphysema but no pneumothorax [Figure - 1] and [Figure - 2]. Bronchoscopy and oesophagoscopy revealed no abnormality. Electrocardiogram showed sinus tachycardia. He was observed in the intensive care unit on 100% oxygen support, and the subcutaneous emphysema gradually resolved over 72 hours. Hamman syndrome (spontaneous pneumomediastinum presenting as subcutaneous emphysema), often idiopathic, is a rare clinical entity. Its incidence is <1:44 000, with a male predominance.[1] Patients can present with thoracic pain, dyspnoea, swelling in the neck, dysphagia, fever or hoarseness of voice. Conservative management is required with follow-up.[2] It is a benign entity with good prognosis. Drainage of subcutaneous air by a microdrainage catheter or skin incisions may be required in symptomatic patients with respiratory distress.
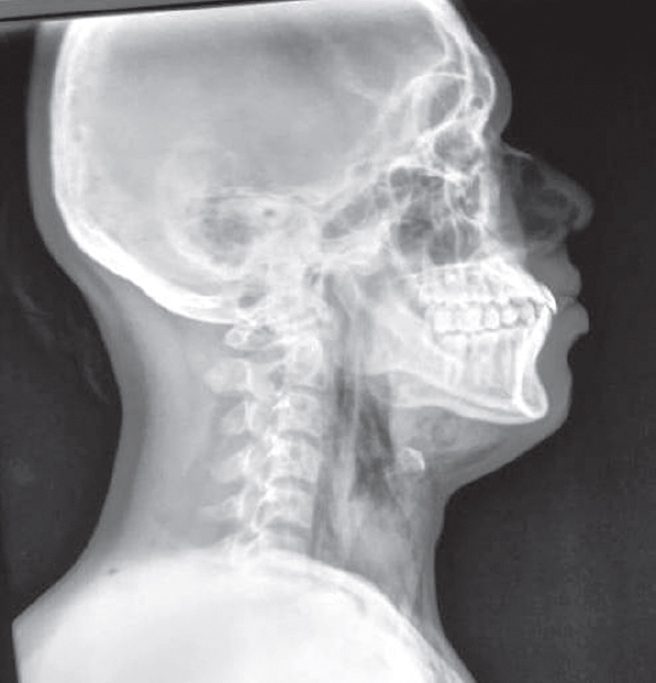 |
| Figure 1: X-ray neck lateral view showing subcutaneous emphysema |
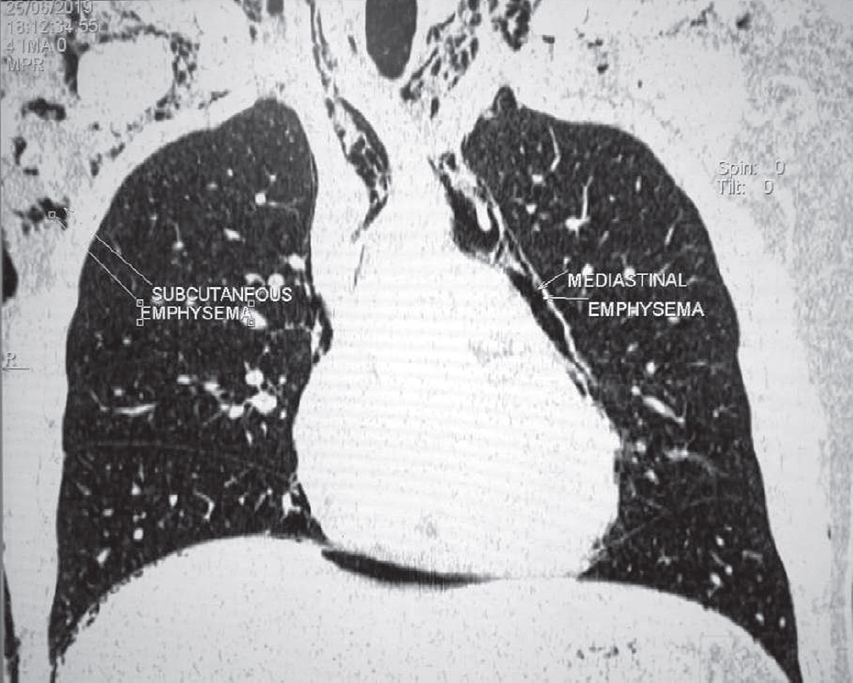 |
| Figure 2: Non-contrast computed tomography chest showing subcutaneous emphysema and pneumomediastinum |
Conflict of interest. None declared
| 1. | Kouritas VK, Papagiannopoulos K, Lazaridis G, Baka S, Mpoukovinas I, Karavasilis V, et al. Pneumomediastinum. J Thorac Dis 2015;7:S44–S49. [Google Scholar] |
| 2. | Jougon JB, Ballester M, Delcambre F, Mac Bride T, Dromer CE, Velly JF, et al. Assessment of spontaneous pneumomediastinum: Experience with 12 patients. Ann Thorac Surg 2003;75:1711–14. [Google Scholar] |
Fulltext Views
1,839
PDF downloads
837




