Translate this page into:
Scoping review of published research on medical education in India during the Covid-19 pandemic
Correspondence to HIMANSHU PANDYA; dr_hvp@yahoo.com
[To cite: Kumar D, Varma J, Dongre A, Pandya H. Scoping review of published research on medical education in India during the Covid-19 pandemic. Natl Med J India 2022;35:243–6.]
Abstract
Background
Medical educators in India made rapid adjustments to maintain continuity and integrity of medical education in the midst of disruption caused by the Covid-19 pandemic. However, there are concerns regarding achievement of competence by undergraduate medical students due to inadequate clinical exposure. We explored the focus of initiatives from medical educators in India by a scoping review of published articles on developments in medical education during the pandemic to map concepts, main sources and the literature available in PubMed.
Methods
We did this scoping review of published articles in PubMed database in four steps: (i) identification of research questions; (ii) identification of relevant studies; (iii) selection of studies meeting inclusion and exclusion criteria, and charting of data; and (iv) collating the summary and reporting of results. Manual content analysis was done to derive frequencies of variables.
Results
Of the 52 articles identified, 22 met the requirements. Most studies (68.2%) were published in 2020. Half of the studies were conducted among undergraduate students and the remaining among postgraduates (27.3%), faculty (18.2%) and interns (4.5%). All the studies were evaluations at Kirkpatrick level-1 (18; 81.8%) and level-2 (4; 18.2%). Most of the studies (9, 41%) focused on exploration of perspectives about online learning among students and faculty, 9 (27.3%) on teaching– learning, 4 (18.2%) on formative assessment and 3 (13.6%) on summative assessment.
Conclusions
Most studies were evaluations at Kirkpatrick level-1 and level-2 among undergraduate medical students with a focus on conceptual understanding.
INTRODUCTION
The objective of medical education is to fashion learners into competent practitioners of medicine, impart medical knowledge and skills, and support professionalism. The Covid-19 pandemic resulted in unparalleled disruption in medical education worldwide including India. Social distancing measures prevented the conduct of classroom teaching and group discussions. Clinical rotations of undergraduate students were halted to avoid risk of exposure to Covid-19 patients.
Medical educators around the world and in India made rapid adjustments in the face of these challenges to maintain the continuity and integrity of medical education. Many have reported their initiatives of online teaching–learning in peer-reviewed journals. Gordon et al. reviewed educational response in the immediate fallout of the pandemic and pointed out lack of practical details and evaluation data in the published literature.1 A recent scoping review of globally published articles on medical education by Daniel et al. identified regional distribution and focus of publications on developments in medical education in response to Covid-19 and offered direction on future developments in online learning.2
Medical educators in India have concerns regarding the implementation of competency-based undergraduate curriculum for medical students admitted since August 2019 and acquisition of clinical competence due to inadequate clinical exposure. Though they have shared their experiences about online medical education through publications, a comprehensive review is lacking. Therefore, we explored the initiatives from medical educators in India by conducting a scoping review of published articles on developments in medical education during the Covid-19 pandemic.
METHODS
Design
We conducted a scoping review to map the concepts, main sources, and the literature available in PubMed to get a broad picture of the developments in medical education in India during the pandemic. An exploratory content analysis approach to the published text articles was adopted.3
Data collection
The scoping review was carried out in four steps by using the York methodology of Arksey and O’Malley.4,5
Identification of research questions. The purpose of the review was pre-defined as stated above.
Identification of relevant studies. Original articles were selected from PubMed with the assumption of quality and rigour in the journals indexed with PubMed. The following search strategy was used: ((“medical education”[All Fields]) AND (“covid”[All Fields])) AND (“India”[All Fields]). Only the articles based on primary data from medical students, interns, postgraduates and faculty were considered for the review.
Selection of studies that met inclusion and exclusion criteria and charting of data. The preliminary review was done by two researchers to ensure trustworthiness. The results of the preliminary review were further appraised by a third researcher. All three researchers have more than a decade of experience in conducting research in medical education.
Collating the summary and reporting of results. A manual content analysis was done using a pre-defined codebook. If any new information emerged, it was adjusted in the framework that was developed in the form of emerging document of codebook. The results are presented as simple frequency for the selected variables.
The institutional ethics committee granted exempt review to this research work.
RESULTS
Of the 52 articles identified in PubMed, full text of 49 articles was obtained.6–55 Of these, 22 articles met the inclusion and exclusion criteria (Fig. 1).
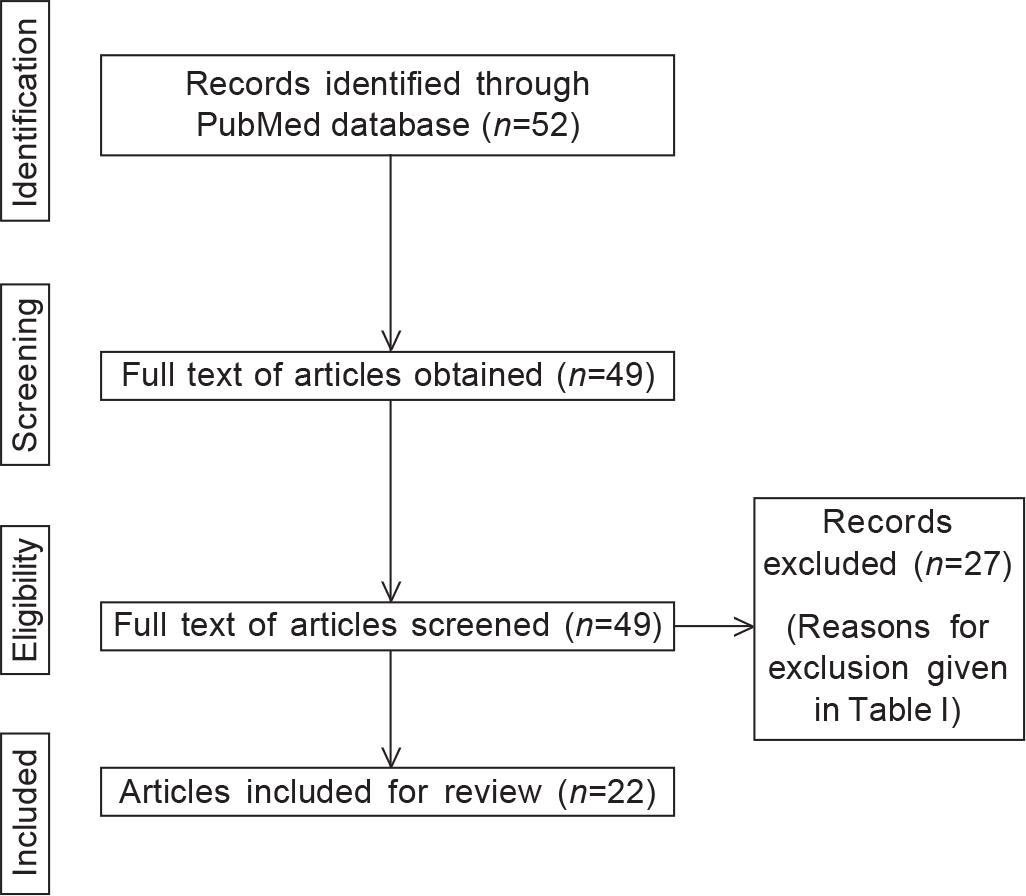
- PRISMA (Preferred reporting items for systematic reviews and meta-analyses) flowchart to show the flow of search results
Most studies (15, 68.2%) were published in the year 2020. Half the studies were conducted among undergraduate medical students and the remaining among postgraduates (27.3%), faculty (18.2%) and interns (4.5%). Half the studies were reported from the northern, 6 (27.3%) from the southern, 3 (13.6%) from the eastern and 2 (9.1%) from the western regions of India. Among 22 studies, 19 (86.4%) used quantitative methods, 2 (9.1%) qualitative methods and only 1 used a mixed-methods approach. All the studies were evaluations at Kirkpatrick level-1 (18; 81.8%) and level-2 (4; 18.2%). Most studies were done in ophthalmology (6, 27.3%), 2 each (9.1%) in anatomy and physiology, and 1 each in neurology, neurosurgery, biochemistry, surgery and preclinical subjects. Five studies (22.7%) targeted undergraduate students across all phases of the MBBS course. Of the 22 studies, 14 (63.6%) were undertaken in government medical colleges, and 6 (27.3%) in private medical colleges. Thirteen (59%) studies used Google form for data collection and 2 (9.1%) used WhatsApp messages. Nine (41%) studies focused on the exploration of perspectives about online learning among students and faculty, 6 (27.3%) on teaching– learning activity (TL activity), 4 (18.2%) on formative assessment and 3 (13.6%) on summative assessment. Among the 6 studies on TL activity, 4 focused on knowledge and 2 on skills assessment. Also, 1 each was based on cognitivism and social-learning theory.
DISCUSSION
We could map the characteristics of various studies on medical education during the Covid-19 pandemic. The results show that medical educators from India adapted to online teaching at a short notice. Most studies were focused on online TL among undergraduate medical students. Medical educators in India mainly used various online and social media platforms. Most of the learning of undergraduate medical students took place in the virtual environment. Among 6 studies on TL activity, 1 each was based on cognitivism and social-learning theories. These findings are consistent with the scoping review by Daniel et al.2
We observed that the studies were not uniformly distributed across various components of curriculum and among the various stakeholders in medical education. Most of the studies were focused on online TL among undergraduate students. During the pandemic, undergraduate medical students in India had their learning experiences mostly through online platforms in settings away from medical schools and different from the workplace in which they will need to apply their learning in future. Since the learning has not happened in authentic clinical setting, all stakeholders would have concerns regarding acquisition of competencies by these batches of future Indian medical graduates (IMG), particularly when medical education in India is undergoing a transition from the traditional to competency-based medical education (CBME).56
It is also evident from the findings of this review that during the pandemic, students who had their education predominantly through online theory classes were deprived of opportunities of not just clinical exposure but also social interaction in authentic clinical settings through the learner–doctor method of clinical training, which would have been possible in normal times. This method of clinical training is based on application of educational theories such as situated learning and communities of practice, which are two interrelated sociocultural frameworks falling under the constructivist paradigm.57
Our review suggests that medical educators in India mainly used various online and social media platforms. Formal learning management systems (LMS) are considered better as they offer space for creating and sharing learning resources as well as a flexible learning environment. LMS also enable tracking of the learner’s and the teacher’s virtual footprints, and thereby curriculum evaluation.58 A judicious blending of informal and formal LMS could enhance learning during normal times by using a hybrid of online and offline education.
Most studies were quantitative in nature as is the trend in medical educational research in India. All the studies in this review were evaluations and mostly at Kirkpatrick level-1. As the evaluations happened during the initial 16 months of the pandemic, the authors perhaps could not progress their studies to higher levels of evaluation.
It is likely that our study being based on articles from a single electronic database, might have missed developments reported by medical educators in other databases. It is also possible that several important developments initiated during the pandemic might not have been published at the time of our review. Though our study was based on articles from only one electronic database, the consistency of findings with the global study indicates its transferability to a similar context.
| Domain | Indicator | Frequency |
|---|---|---|
| Year of publication | 2020 | 15 (68.2) |
| 2021 (till May 2021) | 7 (31.8) | |
| Target group | Undergraduate | 11 (50) |
| Intern | 1 (4.5) | |
| Postgraduate | 6 (27.3) | |
| Faculty | 4 (18.2) | |
| Region | Northern | 11 (50) |
| Southern | 6 (27.3) | |
| Eastern | 3 (13.6) | |
| Western | 2 (9.1) | |
| Northeastern | 0 (0) | |
| Type of evaluation study design | Qualitative | 2 (9.1) |
| Quantitative | 19 (86.4) | |
| Mixed-methods | 1 (4.5) | |
| Kirkpatrick level of evaluation study | Level-1 | 18 (81.8) |
| Level-2 | 4 (18.2) | |
| Subject (specialty) | Anatomy | 2 (9.1) |
| Physiology | 2 (9.1) | |
| Ophthalmology | 6 (27.3) | |
| Neurology | 1 (4.5) | |
| Neurosurgery | 1 (4.5) | |
| Biochemistry | 1 (4.5) | |
| Surgery | 1 (4.5) | |
| Preclinical subjects | 1 (4.5) | |
| Otorhinolaryngology | 1 (4.5) | |
| All subjects undergraduate students | 5 (22.7) | |
| Clinical subjects | 1 (4.5) | |
| Type of organization | Government | 14 (63.6) |
| Private | 6 (27.3) | |
| Non-governmental organization | 1 (4.5) | |
| Multicentric | 1 (4.5) | |
| Online platform used (multiple responses) | G suite | 1 (4.5) |
| Google form | 13 (59) | |
| 2 (9.1) | ||
| 1 (4.5) | ||
| Cisco web | 1 (4.5) | |
| Video conferencing | 1 (4.5) | |
| Go To Webinar | 1 (4.5) | |
| Zoom | 1 (4.5) | |
| Moodle | 1 (4.5) | |
| Cloud-based link | 1 (4.5) | |
| Focus of the study (multiple response) | Exploration of perspectives (students/faculty) | 9 (40.9) |
| Experience sharing | 1 (4.5) | |
| Knowledge, attitude and practice survey | 2 (9.1) | |
| Teaching and learning | 6 (27.3) | |
| Formative assessment | 4 (18.2) | |
| Summative assessment | 3 (13.6) | |
| If teaching and learning, then specify (n=6) | Knowledge | 4 (67) |
| Skills | 2 (33) | |
| Attitudes | 0 (0) | |
| Reasons for exclusion of article (n=27) | Review article | 12 (44.4) |
| Other country | 4 (14.8) | |
| Letter to editor | 5 (18.5) | |
| Not relevant to medical education | 6 (22.2) |
Conclusions and recommendations
During the Covid-19 pandemic, medical educators in India could quickly adapt and ensure cognitive learning of students through online platforms away from authentic settings. Future research in this area should include a systematic review, preferably focused on educational outcomes of the innovations during the pandemic reported in multiple databases. To meet the challenges of creating real-life situations in virtual settings, a blending of informal and formal LMS could be continued even during normal times.
References
- Developments in medical education in response to the COVID-19 pandemic: A rapid BEME systematic review: BEME Guide No. 63. Med Teach. 2020;42:1202-15.
- [CrossRef] [PubMed] [Google Scholar]
- An update on developments in medical education in response to the COVID-19 pandemic: A BEME scoping review: BEME Guide No. 64. Med Teach. 2021;43:253-71.
- [CrossRef] [PubMed] [Google Scholar]
- What are scoping studies? A review of the nursing literature. Int J Nurs Stud. 2009;46:1386-400.
- [CrossRef] [PubMed] [Google Scholar]
- Building collaboration: A scoping review of cultural competency and safety education and training for healthcare students and professionals in Canada. Teach Learn Med. 2017;29:129-42.
- [CrossRef] [PubMed] [Google Scholar]
- Medical education amid the COVID-19 pandemic. Indian Pediatr. 2020;57:652-7.
- [CrossRef] [PubMed] [Google Scholar]
- Medical education during the COVID-19 pandemic: A single institution experience. Indian Pediatr. 2020;57:678-9.
- [CrossRef] [PubMed] [Google Scholar]
- Anatomy education of medical and dental students during COVID-19 pandemic: A reality check. Surg Radiol Anat. 2021;43:515-21.
- [CrossRef] [PubMed] [Google Scholar]
- Moving towards online rheumatology education in the era of COVID-19. Clin Rheumatol. 2020;39:3215-22.
- [CrossRef] [Google Scholar]
- Impact of COVID-19 on medical education: Introducing homo digitalis. World J Urol. 2021;39:1997-2003.
- [CrossRef] [PubMed] [Google Scholar]
- Forensic undergraduate education during and after the COVID-19 imposed lockdown: Strategies and reflections from India and the UK. Forensic Sci Int. 2020;316:110500.
- [CrossRef] [PubMed] [Google Scholar]
- The pedagogical shift during COVID 19 pandemic: Online medical education, barriers and perceptions in central Kerala. J Med Educ Curric Dev. 2020;7:2382120520951795.
- [CrossRef] [PubMed] [Google Scholar]
- The impact of COVID-19 related lockdown on ophthalmology training programs in India; Outcomes of a survey. Indian J Ophthalmol. 2020;68:999-1004.
- [CrossRef] [PubMed] [Google Scholar]
- Education, training, and practices of neurorehabilitation in India during the COVID-19 pandemic. Front Neurol. 2021;12:626399.
- [CrossRef] [PubMed] [Google Scholar]
- Medical education during COVID-19 associated lockdown: Faculty and students' perspective. Med J Armed Forces India. 2021;77(Suppl 1):S79-S84.
- [CrossRef] [PubMed] [Google Scholar]
- Where does Indian medical education stand amidst a pandemic? J Med Educ Curric Dev. 2020;7:2382120520951606.
- [CrossRef] [PubMed] [Google Scholar]
- Online medical education in India: Different challenges and probable solutions in the age of COVID-19. Adv Med Educ Pract. 2021;12:237-43.
- [CrossRef] [PubMed] [Google Scholar]
- Education in times of COVID-19 pandemic: Academic stress and its psychosocial impact on children and adolescents in India. Int J Soc Psychiatry. 2021;67:397-9.
- [CrossRef] [PubMed] [Google Scholar]
- Medical education during the COVID-19 pandemics: Challenges ahead. Indian Pediatr. 2020;57:772.
- [CrossRef] [PubMed] [Google Scholar]
- Neurosurgery training in India during the COVID-19 pandemic: Straight from the horse's mouth. Neurosurg Focus. 2020;49:E16.
- [CrossRef] [PubMed] [Google Scholar]
- Available videoconferencing freeware and medical education. Ind Psychiatry J. 2020;29:155-8.
- [CrossRef] [PubMed] [Google Scholar]
- Trainee education during COVID-19. Neuroradiology. 2020;62:1057-8.
- [CrossRef] [PubMed] [Google Scholar]
- Online medical teaching in COVID-19 era: Experience and perception of undergraduate students. Maedica (Bucur). 2020;15:440-4.
- [Google Scholar]
- Virtual postgraduate orthopaedic practical examination: A pilot model. Postgrad Med J. 2021;97:650-4.
- [Google Scholar]
- A survey of E-learning methods in nursing and medical education during COVID-19 pandemic in India. Nurse Educ Today. 2021;99:104796.
- [CrossRef] [PubMed] [Google Scholar]
- Medical doctors in India are on strike: A moral and national conundrum. Postgrad Med J. 2022;98:313-14.
- [CrossRef] [PubMed] [Google Scholar]
- Assessment of online teaching as an adjunct to medical education in the backdrop of COVID-19 lockdown in a developing country: An online survey. Indian J Ophthalmol. 2020;68:2399-403.
- [CrossRef] [PubMed] [Google Scholar]
- COVID-19 pandemic: Testing times for post graduate medical education. Indian J Ophthalmol. 2021;69:157-8.
- [CrossRef] [PubMed] [Google Scholar]
- Efforts to cope with CBME in COVID-19 era to teach biochemistry in medical college. Biochem Mol Biol Educ. 2020;48:670-4.
- [CrossRef] [PubMed] [Google Scholar]
- Utility of real-time online teaching during COVID era among surgery postgraduates. Indian J Surg. 2020;82:762-8.
- [CrossRef] [PubMed] [Google Scholar]
- Post-graduate exams amidst COVID-19 pandemic: Our experience. Indian J Ophthalmol. 2020;68:2630-1.
- [CrossRef] [PubMed] [Google Scholar]
- COVID-19 and the medical education system in ophthalmology:Lessons learned and future directions. Indian J Ophthalmol. 2021;69:1332-3.
- [CrossRef] [PubMed] [Google Scholar]
- Virtual dermatopathology: A potential educational tool during COVID-19 pandemic. Dermatol Ther. 2020;33:e13755.
- [CrossRef] [Google Scholar]
- Perception among ophthalmologists about webinars as a method of continued medical education during COVID-19 pandemic. Indian J Ophthalmol. 2021;69:951-7.
- [CrossRef] [PubMed] [Google Scholar]
- Rapid transition to online practical classes in preclinical subjects during COVID-19: Experience from a medical college in North India. Med J Armed Forces India. 2021;77(Suppl 1):S161-S167.
- [CrossRef] [PubMed] [Google Scholar]
- Surgical training “Before COVID-19 (BC)” to “After COVID-19 (AC)”: Needs-driven approach for the global South. Br J Surg. 2020;107:e585-e586.
- [Google Scholar]
- Perspectives of physicians regarding the role of webinars on medical education during the COVID-19 pandemic. Indian J Ophthalmol. 2021;69:1251-6.
- [CrossRef] [PubMed] [Google Scholar]
- What is lost in postgraduate residency during COVID-19 Times?--a resident perspective on diagnostic error. Med Sci Educ. 2020;30:1339-40.
- [CrossRef] [PubMed] [Google Scholar]
- A validated audio-visual educational module on examination skills in ophthalmology for undergraduate medical students in the COVID-19 season--An observational longitudinal study. Indian J Ophthalmol. 2021;69:400-5.
- [CrossRef] [PubMed] [Google Scholar]
- Online MD pediatrics exit examination: A novel method of end curriculum summative assessment amidst the ongoing COVID-19 pandemic. Indian Pediatr. 2020;57:1089.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of undergraduate medical students' preference to human anatomy practical assessment methodology: A comparison between online and traditional methods. Surg Radiol Anat. 2021;43:531-5.
- [CrossRef] [PubMed] [Google Scholar]
- Medical students' perception of the reliability, usefulness and feasibility of unproctored online formative assessment tests. Adv Physiol Educ. 2021;45:84-8.
- [CrossRef] [PubMed] [Google Scholar]
- Impact of ophthalmic webinars on the resident's learning experience during COVID-19 pandemic: An insight into its present and future prospects. Indian J Ophthalmol. 2021;69:145-50.
- [CrossRef] [PubMed] [Google Scholar]
- Embracing the change: Resuming advanced trauma training in the COVID-19 era. Med J Armed Forces India. 2021;77(Suppl 1):S140-S145.
- [CrossRef] [PubMed] [Google Scholar]
- Blended programmatic assessment for competency based curricula. J Postgrad Med. 2021;67:18-23.
- [CrossRef] [PubMed] [Google Scholar]
- Wetlab training during COVID-19 era; An ophthalmology resident's perspective. Indian J Ophthalmol. 2021;69:158-9.
- [CrossRef] [PubMed] [Google Scholar]
- Medical education in the midst of a pandemic: What are the longer term consequences for the doctors of tomorrow? Med J Armed Forces India. 2021;77(Suppl 1):S4-S7.
- [CrossRef] [PubMed] [Google Scholar]
- Online open-book examination of undergraduate medical students--a pilot study of a novel assessment method used during the coronavirus disease 2019 pandemic. J Laryngol Otol. 2021;135:288-92.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of e-OSPE as compared to traditional OSPE: A pilot study. Biochem Mol Biol Educ. 2021;49:457-63.
- [CrossRef] [PubMed] [Google Scholar]
- Emergency remote learning in anatomy during the COVID-19 pandemic: A study evaluating academic factors contributing to anxiety among first year medical students. Med J Armed Forces India. 2021;77(Suppl 1):S90-S98.
- [CrossRef] [PubMed] [Google Scholar]
- Online group cognitive behavioral therapy for panic buying: Understanding the usefulness in COVID-19 context. Indian J Psychiatry. 2020;62:607-9.
- [CrossRef] [PubMed] [Google Scholar]
- Efficacy of an online course in developing competency for prescribing balanced diet by medical students: A non-inferiority trial. Indian J Public Health. 2021;65:51-6.
- [CrossRef] [PubMed] [Google Scholar]
- Online teaching in medical training: Establishing good online teaching practices from cumulative experience. Int J Appl Basic Med Res. 2020;10:149-55.
- [CrossRef] [PubMed] [Google Scholar]
- Effects of the COVID-19 pandemic on the competency of clinical year medical students, with special reference to community and public health. Am J Public Health. 2021;111:378-9.
- [CrossRef] [PubMed] [Google Scholar]
- Global health education amidst COVID-19: Disruptions and opportunities. Ann Glob Health. 2021;87:12.
- [CrossRef] [PubMed] [Google Scholar]
- National Medical Commission. Available at www.nmc.org.in/ActivitiWebClient/open/getDocument?path=/Documents/Public/Portal/Gazette/GME-06.11.2019.pdf (accessed on 24 Aug 2021)
- [Google Scholar]
- Situated learning: Legitimate peripheral participation. Cambridge:Cambridge University Press; 1991
- [CrossRef] [Google Scholar]
- Curriculum delivery in medical education during an emergency: A guide based on the responses to the COVID-19 pandemic. Med Ed Publish 2020:9.
- [CrossRef] [Google Scholar]




