Translate this page into:
Total penile necrosis as a manifestation of catastrophic antiphospholipid syndrome
Corresponding Author:
Najib Kachouh
Department of Plastic Surgery, Hôpital de la Conception, Hôpitaux de Marseille Aix-Marseille University, Marseille
France
najib.kachouh@gmail.com
| How to cite this article: Kachouh N, Philandrianos C, Bertrand B, Casanova D. Total penile necrosis as a manifestation of catastrophic antiphospholipid syndrome. Natl Med J India 2018;31:309 |
The occurrence of priapism in systemic diseases is exceptional. It has been reported with Behcet disease, Henoch-Schonlein purpura, Crohn disease, ulcerative colitis and Kawasaki disease.[1] Venous thromboembolism is one of many possible causes of priapism.[1] A 19-year-old man was initially admitted to a regional hospital for management of inflammatory arthritis of the ankle associated with low-grade fever and digestive disorders. Because of an unexpected acute priapism evolving for 4 hours, he was sent to the emergency room. The corpora cavernosa was punctured without much improvement. Four hours later, the situation evolved into an ‘eggplant’ penis. A second puncture of the corpora cavernosa under general anaesthesia and a sponge-carverno anastomosis Ebbehoj -Lue were done but were unsuccessful. Thrombosis of the cavernous bodies was diagnosed. The evolution was characterized partly by local worsening of the clinical aspect of the penis (total penile necrosis) and then by general worsening of the patient’s clinical conditions: massive expansion of necrotic purpura, mucoid-bloody diarrhoea and respiratory distress. The patient was admitted to the intensive care unit following multiple organ failure due to catastrophic antiphospholipid syndrome, diagnosed by a bioassay of the antiphospholipid antibodies and evocative imagery. CT scan revealed thrombosis of the pelvic vessels and the inferior vena cava, explaining the venous priapism. p-ANCA microscopic polyangiitis was diagnosed by a positive serology for p-ANCA specific to microscopic polyangiitis and a kidney biopsy showing an extra capillary necrotizing glomerulonephritis. Immunosuppression including corticosteroids, cyclosporine and immunoglobulin G was started along with long-term anticoagulation. Once extension of the lesions was stabilized, therapeutic management of the necrosis of the penis and perineum consisted of several debridement procedures leading to total amputation of the penis and the bulbar urethra up to the prostate and loss of deep substance of the perineum. Total urethroplasty with two buccal mucosal grafts was done, along with perineal reconstruction using a pedicle myocutaneous gracilis flap. The perineal wound healed completely 6 months after surgery. The 2-cm long neourethra was continent without a fistula. The immunosuppressive treatment has been discontinued for the past 18 months with no relapse.
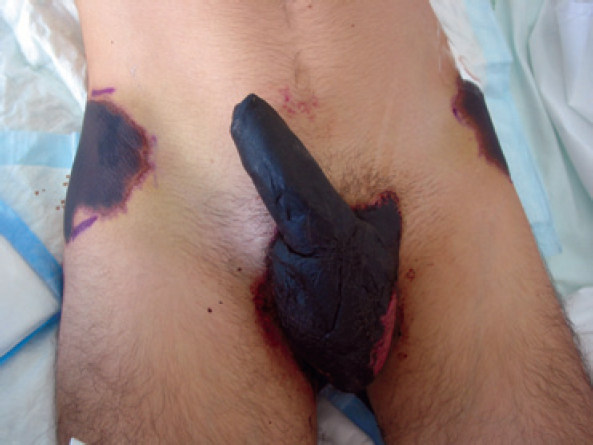 |
| Figure 1: Penile necrosis caused by priapism and necrotic purpura on the hips |
The association between antiphospholipid syndrome and microscopic polyangiitis is rare,[2] since prevalence was 17% for the presence of antiphospholipid antibodies in all-systemic vasculitis.[2] Catastrophic antiphospholipid syndrome or Asherson syndrome affects < 1 % of patients with antiphospholipid syndrome.[3] It is characterized by simultaneous occurrence of multiple thromboses, dominated by their typical microcirculatory fields, which can lead to multiple organ failure. Macroarterial or venous thrombosis can sometimes be associated.[3] This observation adds a new clinical manifestation to catastrophic antiphospholipid syndrome and suggests that cases of unexplained priapism with systemic manifestations should be tested for catastrophic antiphospholipid syndrome and should be promptly managed.
| 1. | Gil H, Magy N, Kleinclauss F, Meaux-Ruault N, Bittard H, Dupond JL. Priapism related to an antiphospholipid syndrome in a patient with systemic lupus erythematosus. Clin Exp Rheumatol 2006;24:217. [Google Scholar] |
| 2. | Kawakami T, Yamazaki M, Takakuwa Y, Yamada H, Ozaki S, Soma Y. Microscopic polyangiitis associated with antiphospholipid antibodies and immune complex mediated cutaneous vasculitis. Acta Derm Venereol 2010;90:639-41. [Google Scholar] |
| 3. | Costedoat-Chalumeau N, Arnaud L, Saadoun D, Chastre J, Leroux G, Cacoub P, et al. Catastrophic antiphospholipid syndrome. Rev Med Interne 2012;33:194-9. [Google Scholar] |
Fulltext Views
2,242
PDF downloads
543




