Translate this page into:
Hirayama disease
Corresponding Author:
A P Shibeesh
Department of General Medicine, Academy of Medical Sciences, Pariyaram, Kannur, Kerala
India
shibeeshap@yahoo.co.in
| How to cite this article: Valliyot B, Sarosh Kumar K K, Beevi K, Sarin S M, Shibeesh A P. Hirayama disease . Natl Med J India 2016;29:311 |
A 70-year-old man presented with a history of weakness, wasting and deformities affecting both hands and forearms starting 40 years ago. There was no associated history of trauma, neck pain or loss of sensation in either upper limb. Neurological examination revealed flexion deformities of both hands ([Figure - 1]) with weakness and atrophy of the thenar, hypothenar, interossei and forearm muscles along with fasciculations and an action tremor affecting both upper limbs. Magnetic resonance imaging (MRI; [Figure - 2]) revealed focal atrophic changes in the spinal cord at the level of the 4th to 7th cervical vertebrae, with an abnormal signal in the region of the anterior horn cells suggestive of Hirayama disease.
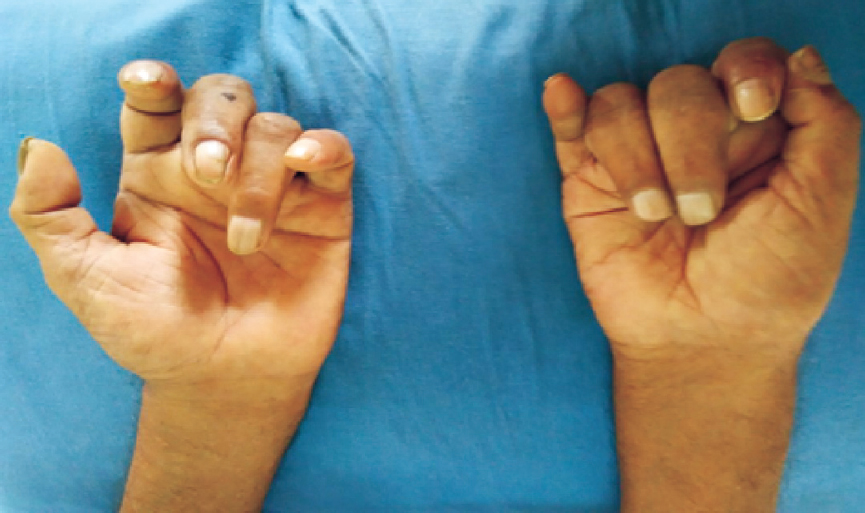 |
| Figure 1. Hands of the patient showing bilateral flexion deformities and wasting of muscles of the forearm |
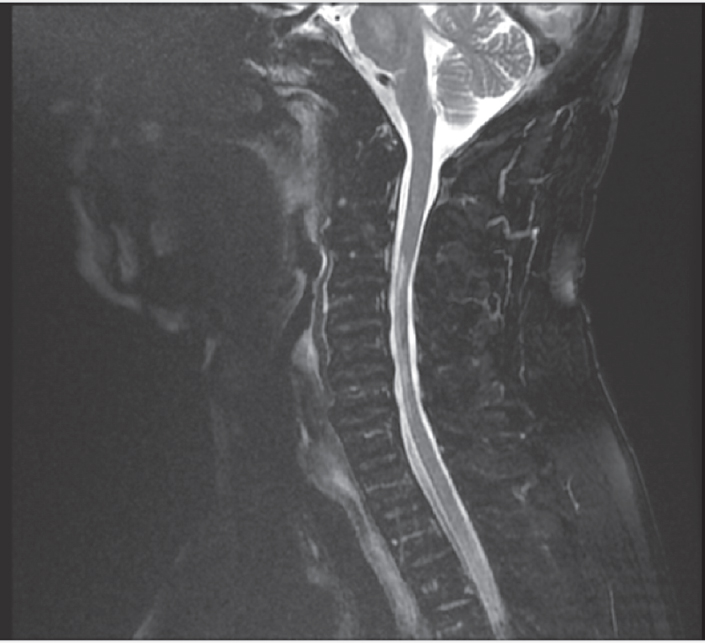 |
| Figure 2. MRI showing thinning of the cervical spinal cord with signal changes in the region of the anterior horn cells |
Hirayama disease typically affects males in the second and third decades with initial progression of weakness and wasting of the distal upper limbs followed by spontaneous arrest of progression after a few years; this distinguishes it from motor neuron disease, which is relentlessly progressive. Syringomyelia, spinal cord tumours, multifocal motor neuropathy and toxic neuropathies are important differential diagnoses. Early in the course of the disease imaging reveals flattening of the spinal cord in routine non-flexion MRI images. In later stages, there may be focal spinal cord atrophy. [1] In the absence of specific treatment, use of a cervical collar and physiotherapy were advised for our patient.
| 1. | Chen CJ, Chen CM, Wu CL, Ro LS, Chen ST, Lee TH. Hirayama disease: MR diagnosis. AJNR Am J Neuroradiol 1998; 19: 365-8. [Google Scholar] |
Fulltext Views
3,187
PDF downloads
1,219




