Translate this page into:
Letter from Ganiyari
Corresponding Author:
Anup Agarwal
Jan Swasthya Sahyog, HEAL Initiative, 298-A Bagmari Road, Raintree Apt, Flat 2C, 2nd Floor, Kolkata 700054, West Bengal
India
mailanupagarwal@gmail.com
| How to cite this article: Agarwal A. Letter from Ganiyari. Natl Med J India 2017;30:294-295 |
Neglected Communities
Last time I thought of diphtheria, it was over 10 years ago. Every medical student reads about diphtheria and is tested on it extensively in multiple-choice questions, short answers and viva voce. I had never seen the disease and believed that I would possibly never see it in this lifetime. Yet, on my first morning at Jan Swasthya Sahayog (JSS), Ganiyari, I woke up to the news that a child with diphtheria had been admitted at night. I masked up and there, lying in the isolation room, I saw a beautiful young girl, lying helpless on a bed with a neck so swollen that it has been apathetically named bull neck. I was excited to see the pseudomembrane in the oropharynx [Figure - 1], diphtheria's cardinal manifestation. My initial excitement gave way to a sense of distress and sadness as I watched this child suffering from a deadly disease. A disease that existed in textbooks but was so forgotten that getting the right medications for diphtheria was a Herculean task.[1]
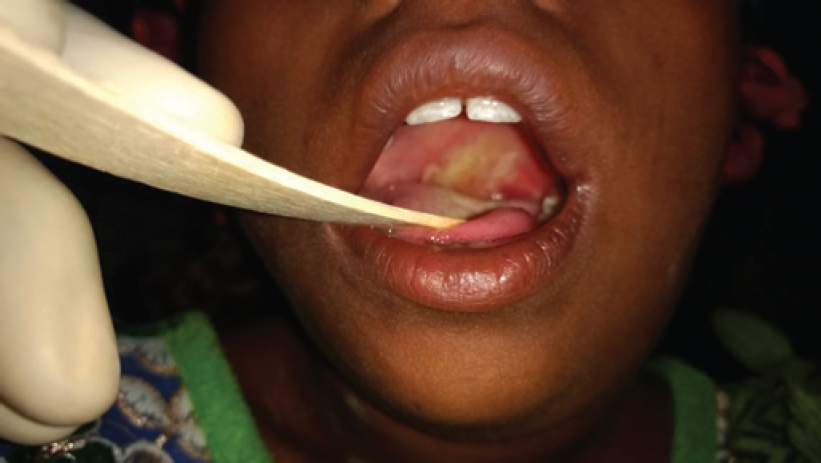 |
| Figure 1: Pseudomembrane of diphtheria |
I then headed over to the emergency room (ER) to start my first shift after completing my residency in internal medicine. A patient with snake bite was being treated by the junior resident and a group of nursing students. The patient was a young farmer who had gone to work in his farm in the morning and ended up in a hospital bed after having a probable life-threatening encounter. The swollen, bleeding and denuded site of the bite was so petrifying that it could leave an imprint on the sufferer's psyche for a lifetime. Thankfully, the junior residents and nurses at JSS were skilled to manage snake bites[2] and the patient went home later that day.
While I was still thinking about the girl with diphtheria and trying to read about the management of snake bites, a couple walked in the ER with a 3 -year-old child in the father's arms. The father told us that the boy had been sick for the past 3 days. He had taken him to a local doctor but his condition had been worsening despite medications. The child was crying, thrashing his limbs, his skin was tomato red and warm to touch. We called our mentor for guidance about the management of this sick-appearing child. He diagnosed the child with Staphylococcal scalded skin syndrome, a life-threatening condition that evolves rapidly and can manifest as blister formation and separation of skin layers. Fortunately, the child received antibiotics promptly and went to a good recovery.
The junior resident then turned my attention to an elderly man, probably in his mid-fifties who had come for evaluation of wounds on his lower extremities, which started 2 weeks ago. He was frail and thin, his shirt was torn and his lungi (waistcloth) was stained with pus. He lay on the bed in a nonchalant manner with no complaints at all about his wounds. On removing the cotton from his wounds, we saw a smattering of ulcers—some superficial and some deep, present circumferentially at the base of his feet but sparing the soles [Figure - 2]. The ulcers were covered with dark dead tissue at some spots, some had pus and others had blood. We asked him how his skin ulcers progressed. He told us that these started as blisters, later ruptured to give it the current appearance. He exposed his hands, where he started noticing similar blisters. We did not have a clue about his condition, but based on our limited understanding of the human body and its various pathologies, we formulated a plan that we believed would help heal his body.
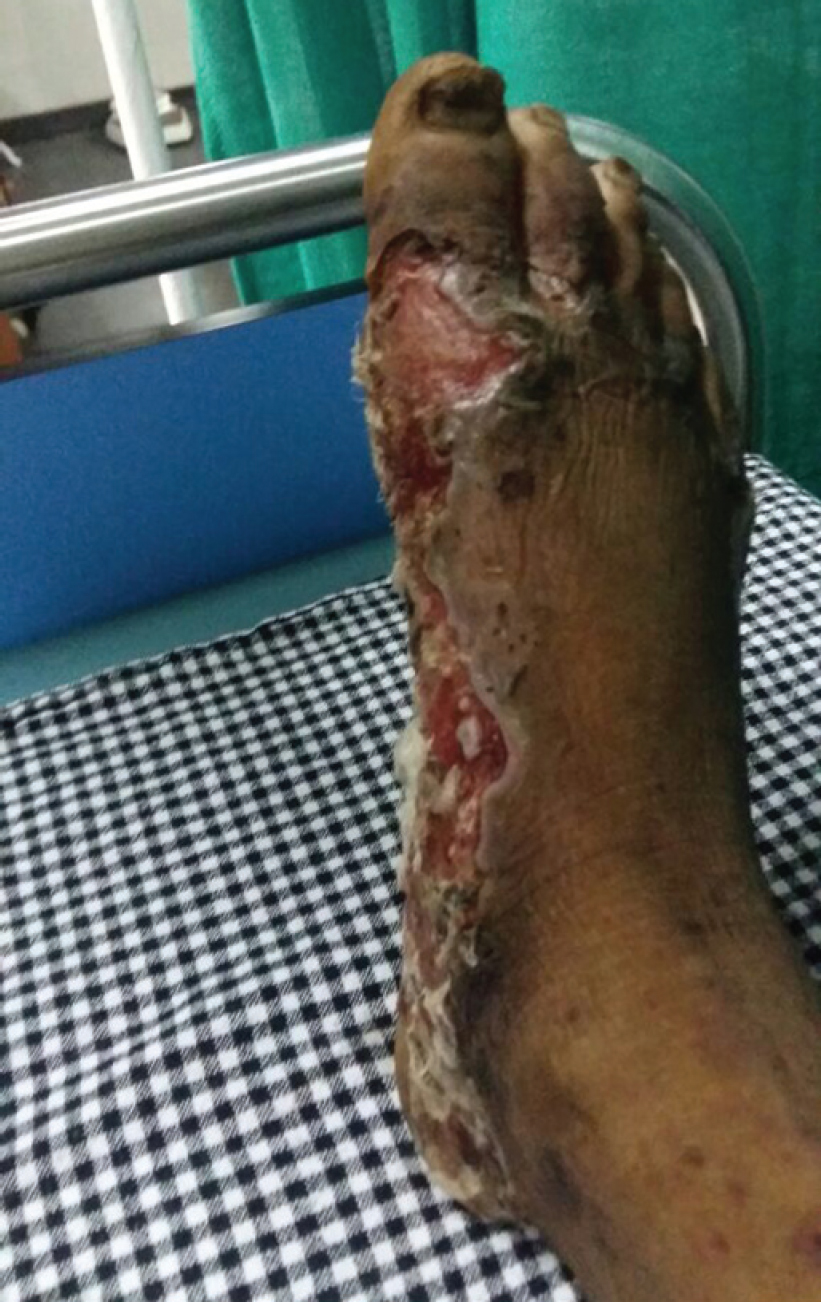 |
| Figure 2: Ulcers circumferentially at the base of the feet |
Struggling to manage patients with my limited knowledge, and minimal resources, I next saw a child lying on one of the beds. He appeared drowsy and was breathing so fast as if he had just completed a 100 m sprint. We suspected pneumonia and started him on the appropriate treatment as we were waiting for the confirmatory chest X-ray. His parents were a young couple, in their twenties. They were frantic and worried and expressed how their child had always been healthy and how much they loved him. The child's condition deteriorated rapidly despite all our efforts. In the next 1 hour, he was intubated and admitted to the high dependency unit.
Finally, the nurse told me that a young man with hydronephrosis had just come into the ER. I told myself, ‘Finally! This is something that I can take care of and went to meet him. He was young, just 28 years old, his face was swollen and puffy, but the rest of his body looked emaciated. He did not respond to any of my questions. His family members said that he had impaired hearing since the age of 16 years and they had never consulted a doctor for it. His younger brother said that he had been ill for the past 3 years, had lost 20 kg in the past 6 months and was delirious for the past 2 weeks. His brother also said that the local tertiary care hospital did not provide adequate treatment to the patient 3 years ago, which, he surmised, had led to the current situation. After completing our assessment, we realized that he had tuberculosis in his kidney and testicles, which had caused his kidneys to fail. Feeling helpless, because of our inability to provide haemodialy sis, we referred him back to the tertiary care hospital, which had probably let him down 3 years ago.
We then went to the high dependency unit to follow up on the child we had admitted. He was intubated, sedated and placed on the ventilator on maximal support. We consulted some of the top experts in the country and abroad. Despite our best efforts, the child died within 24 hours of being admitted. He died because, in rural settings in our country, necessary diagnostic tests are not available and medications and therapeutics are priced out of range or limited in supply. He died because, in rural India, we do not build tertiary care hospitals, we do not build paediatric ICUs and we do not have adequately skilled physicians. The father took the baby home. We, including our society at large, failed that family.
It was my first time working in such a low-resource setting. The term ‘low-resource setting’ does not represent the inequality or the ordeal that patients suffer and physicians struggle within these settings. I was taught in medical school that bicarbonate is a poor man's acid-base analysis, but what does one do when even serum bicarbonate levels are not available. I would like to rename ‘low-resource settings’ like Ganiyari as ‘neglected communities’. In these communities, the whole universe conspires against the people. Basic necessities such as roti aur kapda (bread and clothing) are a luxury, and makaan (shelter) is human imagination. These communities have not only been neglected by their fellow humans, but it seems the bacteria and viruses are also waging a war against them. Even if we as doctors get vehicles to reach them, the roads are not available; if we get phones to contact them, the networks are not available; and even if we get ventilators, the electricity is not available. Probably, in neglected societies, the people are so overwhelmed with getting through the day that they are nonchalant about suffering from necrotic ulcers on both feet.
| 1. | Jain Y. Persistence of diphtheria in India signals need for accessible drugs for neglected illnesses. Available at www.thewire.in/159002/diphtheria-India-accessibility-drugs-neglected-illnesses/ (accessed on 15 Oct 2017). [Google Scholar] |
| 2. | Jan Swasthya Sahyog. Snake and animal bites. Available at www.jssbilaspur.org/ animal-bites/ (accessed on 15 Oct 2017). [Google Scholar] |
Fulltext Views
1,241
PDF downloads
314




