Translate this page into:
National exit test: The medical faculty perspective—A pilot study
Correspondence to PUJA DULLOO; drpujapsmc@gmail.com
To cite: Dulloo P, Kanitkar M. National exit test: The medical faculty perspective—A pilot study. Natl Med J India 2022;35:28–31.
Abstract
Background
Implementation of the exit examination for medical graduates in India has been debated for many years. The national exit test (NEXT), under the construct of the National Medical Commission Act, would serve two purposes: first, it will be a common exit/licentiate examination for all Indian medical graduates, and second, it will be a test for postgraduate selections for all specialties. There has been no research or evidence on stakeholders’ opinion on this test. We aimed to assess the perspective of medical faculties, nationwide, regarding the implementation of NEXT.
Methods
We conducted a nationwide, cross-sectional, questionnaire-based pilot survey. The Google survey form with close- and open-ended questions was forwarded via email and WhatsApp to various groups.
Results
Two hundred and forty-five medical teachers participated, of which 35.9% were from Gujarat, 44.9% were working in government colleges, 91.43% had MD/MS as the highest professional degree, 50% had >15 years of experience and were from different medical specialties. The majority felt that the NEXT examination was a positive step, 82.5% suggested that a national selection/testing authority should conduct it, 36.3% suggested having the test after internship while 32.7% expected some weightage for each year of the medical programme, and 84.1% agreed that all the learning domains should be assessed by various strategies.
Discussion
Faculties welcomed the NEXT examination under a national testing authority. The necessity of this examination is to have uniform standards and quality for medical graduates irrespective of their institutes. Assessment of all the domains will make the Indian medical graduate more competent for the job or residency programmes.
INTRODUCTION
The exit examination, as the name indicates, can be taken as a last ‘clearance’ before leaving law school and is the term coined for completion of training as a lawyer.1 However, this applies to all other professional courses for example in medicine, it implies becoming a competent physician. The National Medical Licensure Examination has been a core component in every country.2–4 The purpose of conducting the licensure for medical graduates is to ensure that qualified graduates have the knowledge and skills necessary to practise medicine safely and effectively.5
In India, the total number of medical colleges, which are recognized or permitted to implement graduation programme (MBBS), are 533, of which 271 are government colleges and 262 are private colleges.6 The students get admission on merit-cum-choice based on their score in the Undergraduate National Eligibility and Entrance Test (NEET-UG), a national entrance test as per the guidelines of the Medical Council of India (MCI).6 It is impossible for the regulatory body to ascertain that graduates from various colleges are adept in the requisite competencies when examined by different agencies. This is despite having been trained on a common curricular framework provided by the council.
It is felt that there has been a decline in the quality of medical training with the mushrooming of medical colleges and insufficient teachers. Therefore, there is a need to implement strict regulations and norms to ensure that medical graduates are competent to practise. The Ministry of Health and Family Welfare and the erstwhile MCI had proposed a progressive plan for all medical graduates to be assessed by an ‘exit exam’.7–16 This examination aims at ensuring that every medical graduate is competent to practise medicine as a doctor as well as pursue postgraduate (PG) studies.
In August 2019, the Indian Medical Council Act was replaced by the National Medical Commission (NMC) bill.17 The NMC bill envisaged introducing a common final year UG examination called the National Exit Test (NEXT), earlier proposed as ‘exit exam’ by the MCI. The medical fraternity has apprehensions about the ‘exit exam,’ as well as NEXT and has expressed its views on several occasions.15,17,18
The NMC has identified various objectives for the NEXT. The first is to ensure a qualified and skilled Indian medical graduate; the second aim is to permit foreign medical graduates to register with the NMC and practise medicine in India; and the third is to serve as a common eligibility test for admission to PG medical courses in India. This examination will subsequently replace the NEET for PG (NEET-PG).18–20 The perceived impact of this examination and knowledge of the stakeholders or their inputs has not been studied. We did a survey of faculty at various medical colleges.
A newspaper report by the Indian Medical Association-Medical Students Network20 put forth certain suggestions for the NEXT examination as follows:
There will be ‘uniformity’ for MBBS final year part 2 examination dates across all the medical institutes in India, thus helping UGs to prepare for the NEXT with clarity.
The NEXT examination will be conducted twice a year, i.e. in March and April.
Applicants qualifying the first part should be eligible to pursue their internship programme.
The second level examination for NEXT should make the applicant eligible for admission to a PG course as well as practise as a medical practitioner in India.
Level one of the NEXT should be via an online portal.
In case the applicant appears for the examination twice, then the higher of the two marks should be taken into consideration.
Considering that medical college faculty are stakeholders, we decided to seek their views regarding NEXT. This pilot survey aimed to identify the perspective of medical faculty nationwide, regarding the implementation of NEXT specifically in terms of learning domains to be tested and modalities for the same.
METHODS
The study was approved by the Institutional Ethical Committee, Pramukhswami Medical College (PSMC), Karamsad. A cross-sectional, questionnaire-based study was conducted. A self-administered structured Google survey questionnaire form was prepared using close- and open-ended questions, validated by subject experts. The readability index for the questionnaire had the text for the average grade level of about 8 (easily understood by 13- to 14-year-olds). The content validity ratio, after input from six qualified experts for each item for accuracy, was +1 for 9 and 0.61 for 5 items. This was administered to faculty members from various medical colleges in India, to seek their views regarding the conduct of the NEXT to acquire the best outcomes for the desired objectives of the examination.
The participants were intimated about the study in the description box of the Google survey form. Participating in the survey was considered as informed consent by the respondents. All faculty members on the medical educators’ platform as well as other groups from various medical colleges of India were invited to participate in the study.
At 95% confidence interval (CI), the sample size calculated on open Epi software was 382.
The data were analysed by percentage scores of respondents. Complete confidentiality at all levels was maintained. The Google survey form was anonymous, as the faculty or institute name was not sought.
RESULTS
Two hundred and forty-five teachers participated in the survey; 91% (223) of participants were from different states while (22) were from Union Territories. Most participants were from Gujarat state (35.9%), with no participation from Arunachal Pradesh, Jharkhand, Manipur, Mizoram, Nagaland (no medical college in this state), Sikkim and Tripura.
The maximum representation was from government medical colleges (44.9%), and the majority of participants had an MD/MS degree (91.4%) as their highest PG specialty qualification. Most participants had more than 20 years of experience, while 20% had 16–20 years of experience. An almost equal number were from preclinical, paraclinical and clinical specialties (Table I).
| Teaching experience of participants | (%) |
|---|---|
| <10 years | 23 |
| 10–15 years | 27 |
| >15 years | 20 |
| >20 years | 30 |
| Faculty specialty area Preclinical | 30 |
| Paraclinical | 27 |
| Medical and allied | 20 |
| Surgery and allied | 23 |
More than 85% (209) of participants responded in the affirmative to the question: ‘Should there be a common entrance test (NEXT)?’; 8.2% (20) did not feel the need for this examination while 6.5% (16) were not sure. The majority felt the examination needs to be conducted by a national testing authority (Table II); 36.3% of participants felt that the examination needs to be conducted after internship, but 32.7% suggested that results from each MBBS professional should be given due weightage (Table II). Most participants (65%) said that the number of chances provided to a candidate to better his or her score should be <5. However, 25.7% (63) suggested unlimited attempts.
| Variable | Participants, n(%) |
|---|---|
| Who should conduct the national exit text ? | |
| University | 25 (10.2) |
| Medical colleges | 5 (2.04) |
| National selection authorities | 202 (82.45) |
| Any other body/agency | 13 (5.31) |
| Ideal time to conduct the national exit text | |
| Before internship | 35 (14.29) |
| After internship | 89 (36.33) |
| Half before and half after internship | 38 (15.51) |
| Each MBBS year should have some weightage | 80 (32.65) |
| Other options* | 3 (1.22) |
| Components to be assessed in the national exit text | |
| Cognitive domain only | 15 (6.12) |
| Clinical skill domain only | 9 (3.67) |
| Cognitive and clinical skill only | 15 (6.12) |
| All three domains (cognitive, clinical skill and affective) | 206 (84.08) |
The participants identified various cognitive assessment tools for NEXT such as extended multiple-choice questions (MCQs; 55.5%), MCQs (45.7%) and short-answer questions (22%). Six participants (2.4%) suggested problem-based questions, MCQs should be based on comprehension, analysis and reasoning, the test should be as per the broad area such as clinical and non-clinical, and the script concordance test. The participants suggested objective-structured clinical examination (75.1%), direct observation performance (25.7%) and logbook (14.7%) as tools for psychometric assessment. Sixteen participants (6.5%) suggested problem-based questions, MCQs should be based on comprehension, analysis and reasoning, the test should be as per the broad area such as clinical and non-clinical, script concordance test, log-book during the internship programme, computer/simulation based exercises, interviews and mini-clinical examination. The affective domain could be assessed through a situational judgement test (39.4%) and logbook for AETCOM (attitude, ethics and communication) maintained throughout the medical course (31.1%) and some other methods (Fig. 1).
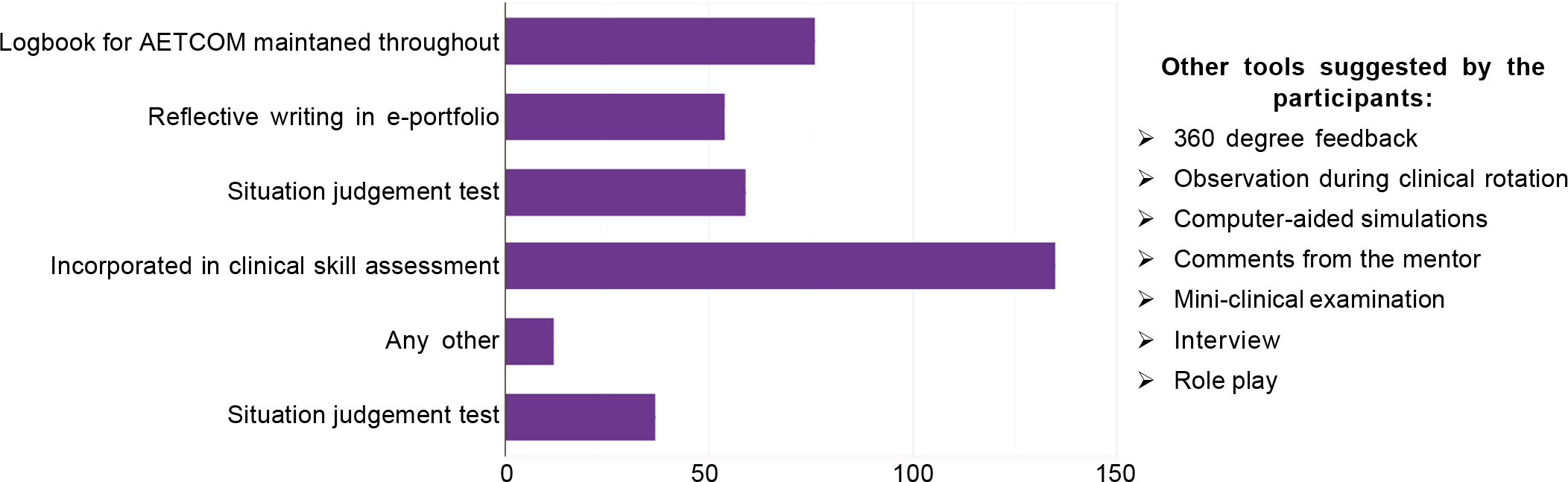
- Tools to assess the affective domain for the national exit test AETCOM attitude, ethics and communication
They further suggested that the NMC may select a panel of examiners or form a central committee of faculty from government medical colleges trained in medical education technology to conduct the clinical skill test for the graduates. As regards the venue for the clinical skills to be assessed, respondents suggested that the examination be conducted at different institutes within the same state. It may be conducted at the PG institutes, or common centres decided by the NMC as is done by the National Board of Examinations for the Diplomate of National Board examination. The students need to be assessed by external examiners.
DISCUSSION
The past decade has witnessed many reforms in medical education in terms of initiating the NEET for UG and PG medical students in India. It has also revised the age-old curriculum and replaced it with a competency-based medical education curriculum.
We focused on the NEXT which is a two-in-one examination for UGs at the end of the MBBS course, providing a medical licence to practise and ranking them for the PG selection test. Although, we are not sure about the content of this examination, we are aware that it will perhaps be held in two phases (steps 1 and 2).21
The Google survey questionnaire form was distributed to over 30 000 medical college faculty members via different e-portals and WhatsApp groups. After three follow-up reminder emails, 245 respondents participated in the study; which is the sample size with a CI of 85%. The reason for inadequate participation could primarily be the busy working schedule of the physicians, where they are occupied in some work (Covid-19 postings or shifting towards online platforms for teaching– learning and assessment strategies) or limited outreach of the survey questionnaire. It is also possible that the faculty were not interested in providing feedback.
More than 85% of participants agreed to a common entrance test for PG selection as the NEXT. Singh et al.22 suggested that Indian medical graduates should undergo an exit test which not only would categorize the institutes but also motivate graduates to be of equal standards, nationally. They have also discussed the pros and cons of the proposed licentiate examination.22 While Dehury and Samal15 specified that the exit test would be a graduate test from the medical college and suggested a minimal impact on improving the standards or the quality of education. Rao23 mentioned that doctors wanted ‘pan-India entrance and exit exams for the medical course’ and that an ‘exit exam can weed out the incompetent doctors.’ While students consider this exit exam as an ‘extra burden’.23 Pardeshi et al.24 have reported that interns wanted a common entrance test.
We found that 82.5% of participants wanted the national selection/testing authorities to conduct NEXT. This will ensure a common national standard with less bias from specific universities and colleges. About 65% of participants considered that the number of attempts should be <5 with the reason that ‘the applicant should not be very old when they enter the PG programme.’ The qualitative open-ended inputs mentioned that ‘customized chances tend to be more efficient and sincere attempts by the candidates,’ ‘anything which is not time-bound is not done,’ ‘as the time passes the performance decreases and adds to frustration.’ Having an unlimited number of attempts was suggested by 25.7% of participants with the reason ‘person is eligible by the talent and not age,’ ‘education and self-improvement should never be limited to a few opportunities,’ ‘improvement in academics should be a continuous process with no restriction on the number of attempts.’ We feel that there should be a limit on the number of attempts, as this may help students take the examination seriously.
Our study shows that 36.3% felt NEXT should be conducted after an internship because ‘there should be a gap of 2 years at least after an internship.’ About 33% felt that each MBBS year should have weightage for this test mentioning that ‘at the end of each professional exam some percentage of marks should be added to the final exam score, throughout the UG.’ While 15.5% felt that half of the examination should be before and another half after an internship because ‘theory should happen before the internship and after 6 months of internship clinical-based exam should be taken,’ ‘1st part basic science should be conducted following completion of phase 2 and 2nd part within 3rd month following completion of internship.’ Mahajan and Singh18 suggested that the exit examination should be conducted while also strengthening the in-course formative assessment. This feedback will provide students an opportunity to improve their skills, communication and attitudes within the duration of the course.
Our study showed that 84.1% of participants agreed to have all the learning domains as a part of the NEXT, which has already been reported.18 However, 6.1% felt it was enough to assess only cognitive and clinical skills. Singh et al.22 mentioned that having a single MCQ-based assessment will not justify how trained the applicant is in terms of clinical skills, communication or affective behaviours. Gliatto et al.25 specified that there is a need to break free of the self-imposed restriction of using a single score for final selection, as it may hamper innovations in medical education to make it relevant to the health requirements of the society. Participants suggested that the NEXT needs to assess all domains of learning. We also believe that there should be multiple ways of assessment since one method may not be able to assess all the competencies. Pardeshi et al.24 reported that 74% of interns agreed to have a clinical skill assessment for the PG selection test. The study suggested having the assessment of skills and the outcome of the internship training, thereby interns would get an opportunity to improve their skills and the same would be helpful for their future practice.24
Pardeshi et al.24 suggested incentives for doctors working in rural areas during the PG selection. Singh et al.22 suggested making the selection more valid by using other tools for testing higher-order thinking skills, aptitude and ethical judgement. The introduction of assessment methods for the affective domain is even more important during NEXT with the newly introduced competency-based curriculum. This will ensure connectivity of UG training programme with that of the selection/ exit examination.
This pilot study has laid the path for further research opportunities. An adequate sample size would strengthen the statistical outcome of the study. Second, faculty from all regions of the country should participate in such a study, to have a national representation of ideas. Lastly, focus group discussion or semi-structured interview could present various opinions from different stakeholders.
Our study has the limitation of a small sample size. Inputs from other stakeholders will add further insight for policy-makers before the NEXT is rolled out.
Conclusion
The introduction of a nationalized exit and PG selection examination is perceived as a good initiative to help standardize the training outcomes of medical graduates irrespective of the university or college. It will help make the Indian medical graduate a globally relevant physician. In spite of the limitation of a small sample size for this survey, it provides an insight into the thought process of the faculty involved in medical education in India. The NEXT is welcomed and it is felt that it needs to assess all the three domains of learning. If the examination is conducted in two parts, the skills need to be assessed after the internship. Weightage may be given to the summative examinations at the end of each part of MBBS. The examination needs to be conducted by a national-level authority rather than a local or regional centre.
ACKNOWLEDGEMENT
We would like to thank all the faculty members who participated in the study.
Conflict of Interest
Dr Madhuri Kanitkar was a member of the Board of Governors in supersession of the Medical Council of India (MCI).
References
- Between closure and opening: Exit exam in Ethiopian law schools––An essay. 2010. Ethiop J Legal Educ. 3:1-25. Available at www.researchgate.net/profile/Tsegaye_Regassa/publication/303459599_Between_Closure_and_Opening_Exit_Exam_in_Law_Schools/links/57442e6508ae9ace841b4aa7/Between-Closure-and-Opening-Exit-Exam-in-Law-Schools.pdf (accessed on 6 Feb 2020)
- [Google Scholar]
- National Board of Medical Examiners 2014. Annual Report. Available at www.nbme.org/PDF/Publications/2014Annual-Report.pdf (accessed on 25 May 2019)
- [Google Scholar]
- General Medical Council. 2014. Available at www.gmc-uk.org/-/media/documents/06___National_Licensing_Examination.pdf_57876215.pdf (accessed on 6 Feb 2020)
- [Google Scholar]
- Undergraduate educational environment, perceived preparedness for postgraduate clinical training, and pass rate on the National Medical Licensure Examination in Japan. BMC Med Educ. 2010;10:35.
- [Google Scholar]
- Search College and Courses. Available at www.mciindia.org/CMS/information-desk/college-and-course-search (accessed on 6 Feb, 2020)
- [Google Scholar]
- IMA opposes MBBS exit exam. 2015. The Times of India TNN. Available at https://health.economictimes.indiatimes.com/news/industry/ima-opposes-mbbs-exit-exam/47730911 (accessed on 6 Feb 2020)
- [Google Scholar]
- Medical exit exam. 2015. The Times of India TNN. Available at https://timesofindia.indiatimes.com/home/education/news/Medical-exit-exam/articleshow/48139259.cms (accessed on 6 Feb 2020)
- [Google Scholar]
- Few takers for MBBS exit exam in state. 2015. The Times of India TNN. Available at timesofindia.indiatimes.com/city/bhopal/Few-takers-for-MBBS-exit-exam-in-state/articleshow/48433540.cms (accessed on 6 Feb 2020)
- [Google Scholar]
- The Hitavada correspondent. MCI clears ‘exit test’ for MBBS pass-outs. The Hitavada.
- [Google Scholar]
- Fresh push for optional exit exam after MBBS. 2015. The Telegraph. Available at www.telegraphindia.com/india/fresh-push-for-optional-exit-exam-after-mbbs/cid/1511755 (accessed on 6 Feb 2020)
- [Google Scholar]
- Govt mulling exit exam for MBBS doctors. India TV News Desk. Available at www.indiatvnews.com/news/exit-exams-for-mbbs-doctors-51139.html (accessed on 6 Feb 2020)
- [Google Scholar]
- A pan-India exit exam proposal for all MBBS doctors. News World India, New Delhi (India). Available at http://blog.santamonica.edu.in/a-pan-india-exit-exam-proposed-for-all-mbbs-doctors/ (accessed on 6 Feb 2020)
- [Google Scholar]
- Govt plans exit exam for MBBS doctors. 2015. The Times of India TNN. Available at https://timesofindia.indiatimes.com/india/Govt-plans-exit-exam-for-MBBS-doctors/articleshow/47494308.cms (accessed on 6 Feb 2020)
- [Google Scholar]
- ‘Exit exams’ for medical graduates: A guarantee of quality? Indian J Med Ethics. 2017;2:190-3.
- [Google Scholar]
- The Economic Times. 2020. Available at https://economictimes.indiatimes.com/news/politics-and-nation/president-ram-nath-kovind-signs-nmc-bill-into-a-law-nmc-to-be-constituted-within-sixmonths/articleshow/70591981.cms?from=mdr (accessed on 3 Jun 2020)
- [Google Scholar]
- The unending debate over ‘exit test’ after MBBS. 2016. Exams Watch Debate Corner, Education News. Available at http://examswatch.com/the-unending-debate-over-exit-test-after-mbbs/ (accessed on 27 Jun 2020)
- [Google Scholar]
- The national licentiate examination: Pros and cons. Natl Med J India. 2017;30:275-8.
- [Google Scholar]
- NEXT (National Exit Test): Exam details for MBBS. 2020. How and when will it be implemented?. Available at www.collegedekho.com/articles/next-national-exit-test-exam-for-mbbs/ (accessed on 3 Jun 2020)
- [Google Scholar]
- NEXT to be become operational within three years students come up with feedback. 2020. Available at www.collegedekho.com/news/next-replace-neet-pg-nmc-bill-16849/ (accessed on 3 Jun 2020)
- [Google Scholar]
- It is time to prepare for NEXT challenges, Hindustan Times. 2020. Available at www.hindustantimes.com/brand-stories/it-s-time-to-prepare-forthe-next-challenge/story-AHMoZWFHGFcf3JBzvApIfN.html (accessed on 11 Jun 2020)
- [Google Scholar]
- Admission to undergraduate and postgraduate medical courses: Looking beyond single entrance examinations. Indian Pediatr. 2017;54:231-8.
- [Google Scholar]
- Doctors differ over exit exam for MBBS graduates. 2018. The Time of India TNN. Available at https://timesofindia.indiatimes.com/city/bengaluru/doctors-differ-over-exit-exam-for-mbbs-graduates/articleshow/62343398.cms (accessed on 9 Aug 2020)
- [Google Scholar]
- MCI and NEET-PG: Understanding the point of view of medical graduates. Natl Med J India. 2012;25:314-15.
- [Google Scholar]
- Scylla and Charybdis: The MCAT, USMLE, and degrees of freedom in undergraduate medical education. Acad Med. 2016;91:1498-500.
- [Google Scholar]




