Translate this page into:
Psychosocial aspects of colour vision deficiency: Implications for a career in medicine
Corresponding Author:
Subho Chakrabarti
Department of Psychiatry, Postgraduate Institute of Medical Education and Research, Sector 12, Chandigarh 160012
India
subhochd@yahoo.com
| How to cite this article: Chakrabarti S. Psychosocial aspects of colour vision deficiency: Implications for a career in medicine. Natl Med J India 2018;31:86-96 |
Abstract
Colour vision deficiency (CVD) is a common problem and persons with CVD experience difficulties in daily life, early learning and development, education, choice of careers and work performance. Medical professionals with CVD also report difficulties in everyday tasks, training in medicine and performance of medical duties. However, because of limited evidence, the real impact of CVD on the lives of medical professionals is unclear, especially regarding the practice of medicine by doctors. The nature and severity of CVD, awareness of its impact, personal circumstances and the ability to cope with the deficiency are the major factors that determine the impact of CVD. However, there is a paucity of methodologically sound research on social and psychological aspects of CVD. Currently, early detection, enhancing awareness and offering support are the only proven ways of helping medical professionals with CVD. With the growing emphasis on equality and inclusivity of those with deficiencies, it is desirable to strike a balance between concerns about patient care and the rights of medical professionals with CVD to pursue their careers. Therefore, any future research also needs to focus on psychological aspects of CVD while exploring its impact on a career in medicine.
Introduction
The impact of colour vision deficiency (CVD) on those intending to pursue a career in medicine has been in the news following the recommendation of a committee appointed by the Supreme Court to remove CVD-related restrictions at all stages of medical education and training.[1] CVD, often wrongly referred to as colour blindness, is a common problem among people including medical professionals. Individuals with CVD experience difficulties in everyday tasks, education and in their careers. However, because of limited evidence, the real impact of CVD on the lives of these people is unclear. The impact of CVD on medical practice is also equally unsettled. Moreover, with the growing emphasis on equal opportunity, it is necessary to strike a balance between concerns about patient care and the rights of doctors with CVD—a principle emphasized by the judgment of the Supreme Court.
CVD Among the General Population
Prevalence and severity
Although a comprehensive review of the aetiology, prevalence and clinical aspects of CVD is beyond the scope of this paper, several important points can be extracted from some reviews on the subject.[2],[3],[4],[5]
Red-green CVD is the most common variety of congenital CVD. It consists of milder or anomalous trichromatic forms (protanomaly or red weakness and deuteranomaly or green weakness) or more severe or dichromatic forms (protanopia and deuteranopia). Other rarer defects include blue-yellow weakness (tritanopia and tritanomaly) and achromatopsia or the complete absence of colour vision. CVD is one of the most common disorders of vision and its congenital form affects about 8% of men and 0.4% of women with North-European ancestry. The gender difference in prevalence results from the red-green type being inherited in an X-linked recessive manner. The influence of a genetic aetiology also makes for varying prevalence rates among different ethnic populations, with rates being lower among Asians, Africans and South Americans. In keeping with this trend, studies from India have found prevalence rates of 2%-4% on average although rates have varied from 1% to 8% across studies.[6],[7],[8],[9],[10]
The extant literature also suggests that total ‘colour blindness’ is extremely rare. Rather, difficulties with colour vision range on a continuum from mild to severe levels of deficiency. When examined for severity, approximately equal numbers of people with red-green forms of CVD are graded as having mild, moderate or severe deficiency.[11] In addition, prevalence studies suggest that only about a quarter of the individuals have a severe form of CVD; the remaining three-quarters may either have normal or near- normal colour vision, or more commonly have a level of ability intermediate between normal colour vision and defective colour vision approaching severe CVD.[2],[3],[4],[12]
Difficulties associated with CVD
CVD affects many areas of life, and its adverse impact is experienced at all stages, i.e. from childhood to adolescence and adulthood.[2],[3],[4],[5],[13],[14] Adverse effects of CVD have been reported mainly in areas of daily living, early learning and development, subsequent educational and occupational performance and other areas such as health-related activities [Table - 1].
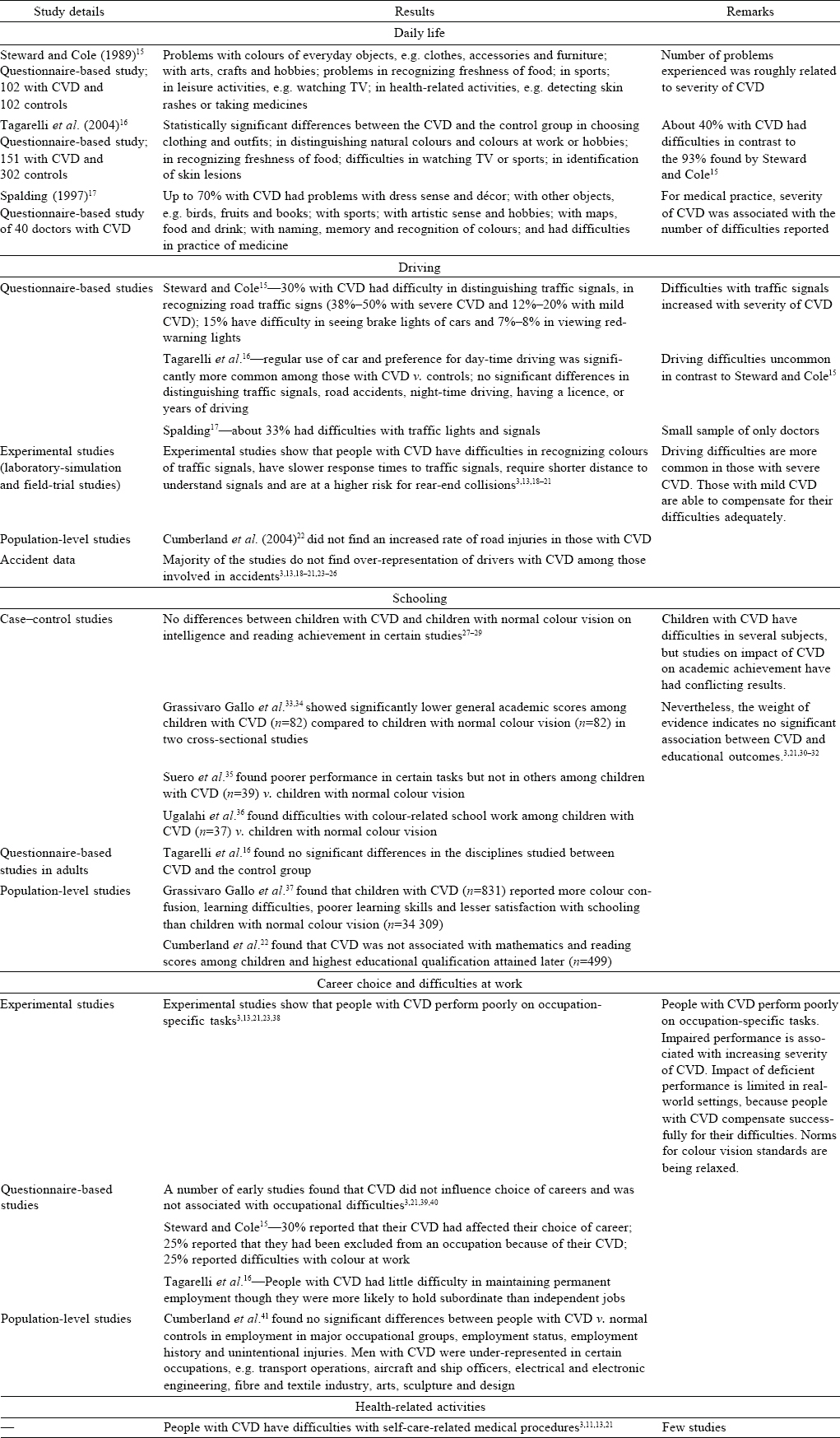
Daily living
The principal tasks where colour is used to organize our daily life are classified into three or four categories.[1113] Comparative colour tasks are those which require matching or differentiating colours, for example in painting or decorating a house, or in textile, paint and plastics industries. Connotative colour tasks are those in which colours are assigned specific meanings that determine the significance of the task. Recognizing traffic signals and other colour-coded information in electrical appliances, chemical tests and colours of eatables are some examples of such tasks. In denotative tasks, colour is used to identify objects or discern complex visual information. These tasks include visual scanning and search to distinguish coloured objects from their background. Aesthetic colour tasks involve the symbolic use of colour to convey ideas or emotions by artists and designers. Since these different uses of colour are common in our daily life, it is not surprising that people with CVD experience problems in daily living. Questionnaire-based studies have shown that a number of people with CVD have problems in negotiating everyday tasks such as driving, cooking, decorating, dressing and sports or leisure activities [Table - 1].[15],[16],[17] However, the proportion of people with difficulties varies from around 40% to 93% in these studies. One factor accounting for this wide range could be the varying severity of CVD.
Driving
Safe driving requires proper recognition of traffic signals, road signs and colour-coded lights. Laboratory-simulation and field trials have shown that drivers with CVD have difficulties in recognizing coloured traffic signals, have slower response times to these signals, require shorter distance to understand signals, have reduced sensitivity to red lights and are at a higher risk for rear-end collisions.[3],[13],[18],[19],[20],[21] The three questionnaire-based studies have come to somewhat different conclusions about driving difficulties of people with CVD.[15],[16],[17] Two of them found that about one-third of the drivers with CVD had various difficulties with traffic signals and other colour signals on the road,[1517] while the third study found no significant differences in distinguishing traffic signals and few differences in other aspects of driving between drivers with and without CVD.[16] Severity of CVD is a confounding factor since driving difficulties are more common in those with severe CVD.[15]·[21] Moreover, drivers can be helped by having to view traffic signals from much shorter distances than maritime, aviation and rail signals. Other environmental cues such as positioning of traffic lights, their relative brightness and movement of other traffic can also help. Specially designed traffic lights and eyeglasses can be of use in certain instances. Finally, those with CVD can compensate for their colour vision deficits by adopting safer and more cautious driving practices.[3],[13],[18],[19],[20],[21] The lack of impact of CVD on driving in natural conditions is endorsed by population-level studies and accident data.[3],[13],[18],[19],[20],[21],[22],[23],[24],[25],[26] More than a dozen studies have examined accident rates among drivers with CVD, with the majority finding no differences between those with or without CVD. Therefore, though CVD is a potential risk factor for driving because of errors in colour-dependent driving tasks, the weight of the evidence indicates that CVD is not associated with unsafe driving.
Schooling and education
Congenital CVD is a hidden disability because, though present from birth, its effects become manifest only when children begin to attend play-schools or regular schools. Since learning from an early age is heavily dependent on colour vision and because CVD is generally not recognized early, it often leads to considerable difficulties in learning. Children with CVD are often labelled as slow learners, which could have adverse psychological impact on them, or could elicit negative reactions from teachers and parents. Young children with CVD have problems in learning, in playing and in the area of personal safety, while older children lag behind in many subjects, especially science subjects.[321] However, the impact of CVD on academic performance remains uncertain because of conflicting findings. While certain cross-sectional controlled studies with relatively smaller samples have found that intelligence and reading ability did not differ between children with CVD and those with normal colour vision, other studies have found school work and academic achievement to be poorer among those with CVD.[16],[27],[28],[29],[30],[31],[32],[33] One large cross-sectional study did find more colour confusion, learning difficulties, poorer learning skills and lesser satisfaction with schooling among children with CVD compared to controls,[37] but another better-designed longitudinal cohort study found that CVD was not associated with mathematics and reading scores among children and the highest educational qualification attained by them at a later age.[22] Therefore, most reviewers have concluded that there is no clear association between CVD and educational outcomes.[3]·[21]·[30] Consequently, there have been calls for abandoning screening at the school-level, and colour vision testing has been largely phased out at school-entry in countries such as the UK.[21]·[22]·[32]
Choice of careers and workplace difficulties
People with CVD have been conventionally debarred from certain occupations because of reasons of safety or lack of quality assurance.[2]·[3]·[21] Occupations requiring normal colour vision to ensure safety include transport, defence and the electronic industries. Occupations requiring surface colours to be recognized or aesthetic judgements about colours to be made, e.g. textile and chemical industries, designing or interior decoration, also exclude those with more severe forms of CVD because of limitations in quality assurance. CVD might create difficulties in other occupations such as teaching, art and medicine, but people with CVD are not usually barred from these fields. Notwithstanding such restrictions, the evidence linking CVD with career choice and workplace difficulties is not clear. Experimental studies show that people with CVD, particularly those with more severe forms, perform poorly on occupation-specific tasks.[3]·[13]·[21]·[23]·[38]·[39] However, the results of questionnaire-based studies are equivocal with some showing CVD to be a determining influence and others failing to do so.[15]·[16]·[40] Moreover, a population-level cohort study found no significant differences between people with or without CVD in employment type, employment status, employment history and risk of workplace injuries.[22]·[41] The lack of evidence clearly linking CVD with occupational difficulties and growing awareness of equal opportunity legislation has meant that many occupations have relaxed their requirements regarding colour vision standards.[2]·[13]·[21]·[38]
Confounding factors
A consistent theme in literature on different difficulties associated with CVD is the discrepancy between the problems linked to CVD found in experimental situations and performance in real-world settings. It is a common finding that laboratory simulations and field trials often do not reflect performance in more natural settings.[13]·[22]·[41]·[42] This is because a number of factors such as existing circumstances, environment, memory and expectation play a role in determining the eventual association between CVD and the difficulties reported in real-life situations. Severity of CVD is another major confounder because it appears to be uniformly associated with the extent of disability in different domains.[13]·[21]·[22]·[38]·[40]·[41] Lack of awareness and denial is also likely to lead to under-reporting of problems and minimization of their seriousness.[12] Finally, people with CVD develop a number of adaptive strategies, consciously or unconsciously, to compensate for their deficiencies. They learn to use other properties of objects such as hue, saturation and brightness or spatial orientation and other environmental clues to successfully overcome their problems.[13]·[22]·[32]·[41] Thus, the results of experimental studies are often not replicated at the population level.[22],[41]
Psychological aspects of CVD
The first description of CVD in 1794 by John Dalton contained a detailed description of its subjective aspects.[13] However, the existing literature on CVD appears to have largely ignored the subjective and psychological aspects of the disability. Since CVD is present from birth, it may hamper early learning and development. Although the findings on school performance are equivocal [Table - 1], the difficulties some children face in school can seriously undermine their confidence and cause frustration and anger.[3]·[32]·[43]·[44] In addition, in young children, the presence of CVD may create difficulties in other areas such as playing, eating or personal safety. These problems are made worse in many instances where the CVD remains undetected for long. Adverse experiences such as these have the potential to affect the child’s self-esteem and more severe problems can even lead to social withdrawal or refusal to go to school. Moreover, trauma resulting from childhood visual impairment can affect self-concept and self-integration at a later age.[45] Thus, adults who have experienced lifelong visual confusion because of CVD may continue to display a range of negative psychological reactions such as frustration, shame and lack of confidence. Grassivaro Gallo et al.[37]have proposed that persons with CVD have difficulty reconciling their own perceptions of reality with those of others. Unawareness of CVD leads them to the conclusion that they are defective and need to change. However, failed attempts at adapting to prevalent norms often result in a sense of lack of control, which in turn leads to helplessness, demoralization, apathy, withdrawal or even rebellion. Impaired self-efficacy and self-esteem are the eventual outcomes of chronic and persistent feelings of helplessness and discouragement. Despite these potential psychological sequelae of CVD, the evidence linking CVD with poor self-esteem or other maladaptive personality traits is meagre and often inconsistent, with psychological difficulties being found only in a few studies [Table - 2].
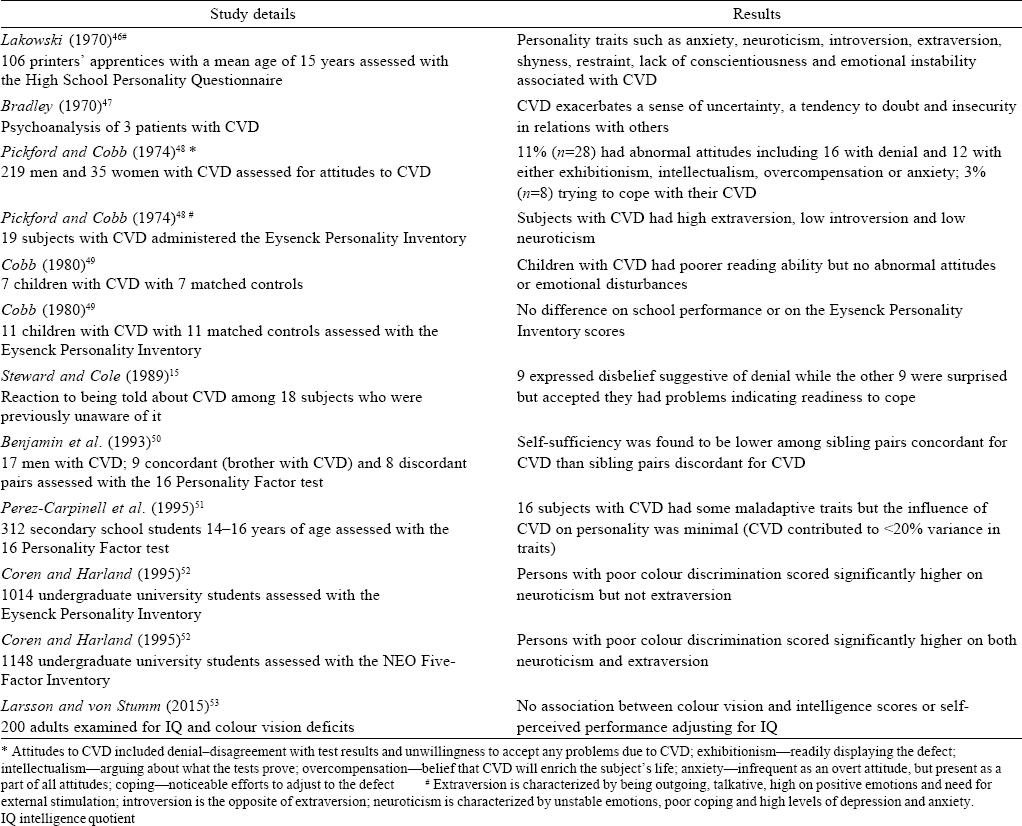
One consistent finding across many studies has been the lack of awareness about the presence and severity of CVD among its sufferers. About one-fifth to one-third of those with CVD do not know about their condition.[5] Steward and Cole[15] found that 25% of those with milder forms of CVD (trichromats) and even 5% with more severe forms (dichromats) were unaware about their CVD. Many people become aware of their CVD only during their school-years. However, despite having their vision checked, 50%-90% of primary schoolchildren remain unaware.[15],[32],[54],[55] Awareness improves during secondary schooling, especially among those with more severe CVD; still, 40%-80% leave school without being aware of their CVD. Awareness among others such as teachers or family members is also low.[7],[32],[37] Unawareness is partly due to the fact that people with CVD might have not been properly tested and informed about their condition. Moreover, they learn to hide their difficulties by adapting to their deficiency using a variety of cues and assumptions to guess the colour of the obj ect they are seeing. Finally, an element of denial is also present [Table - 2]. This often arises from an internal struggle among people with CVD whether to reveal their problems or to hide them to avoid facing discrimination.[11],[12]
CVD And The Medical Profession
Prevalence and severity
The prevalence of CVD among medical workers suggests that those in the medical profession are not immune to problems arising from CVD. The rates of CVD among medical professionals have differed across studies possibly due to methodological discrepancies [Table - 3].[11]·[12]·[57]·[58]·[70] Although rates either lower or higher than that among the general population have been reported, CVD is as common among medical professionals as in other people. Studies on medical students from the Indian subcontinent also show that rates range from 1% to 6%, which is similar to the rates among the general population.
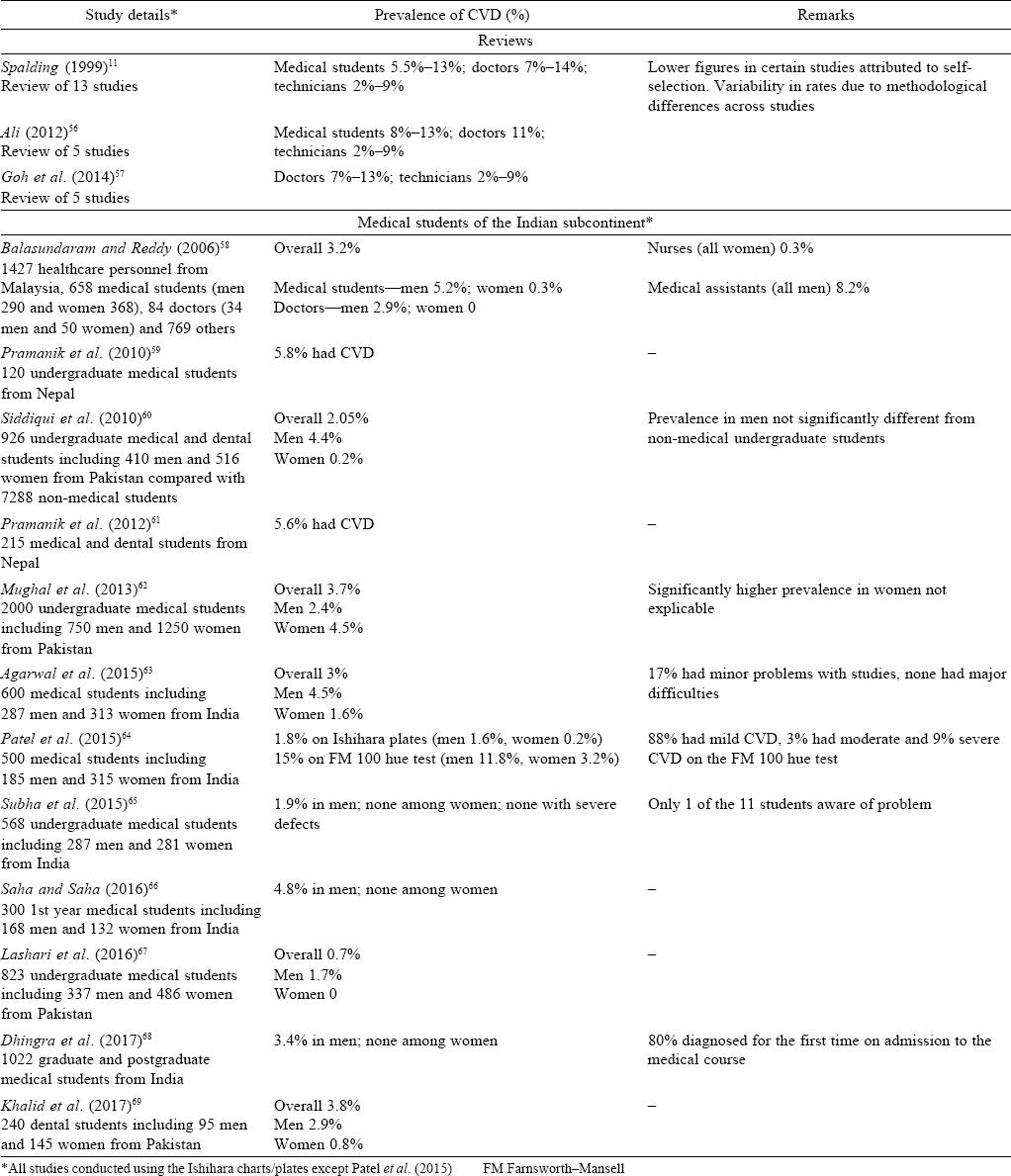
Difficulties associated with CVD
The problems that students and doctors with CVD face while training in and practising medicine have been noted for more than 100 years.[71]·[72] However, possibly because of reluctance of the medical profession to acknowledge these problems, research on this aspect of CVD began in earnest only in the 1990s. Consequently, the evidence is not as extensive or methodologically sound as studies done among the general population. The bulk of evidence consists of studies using colour-dependent material for assessing medical skills of students or doctors in artificial test conditions. This is supplemented by a few questionnaire-based studies, direct observations of doctors while performing medical procedures and subjective accounts of their difficulties due to CVD Table 4].
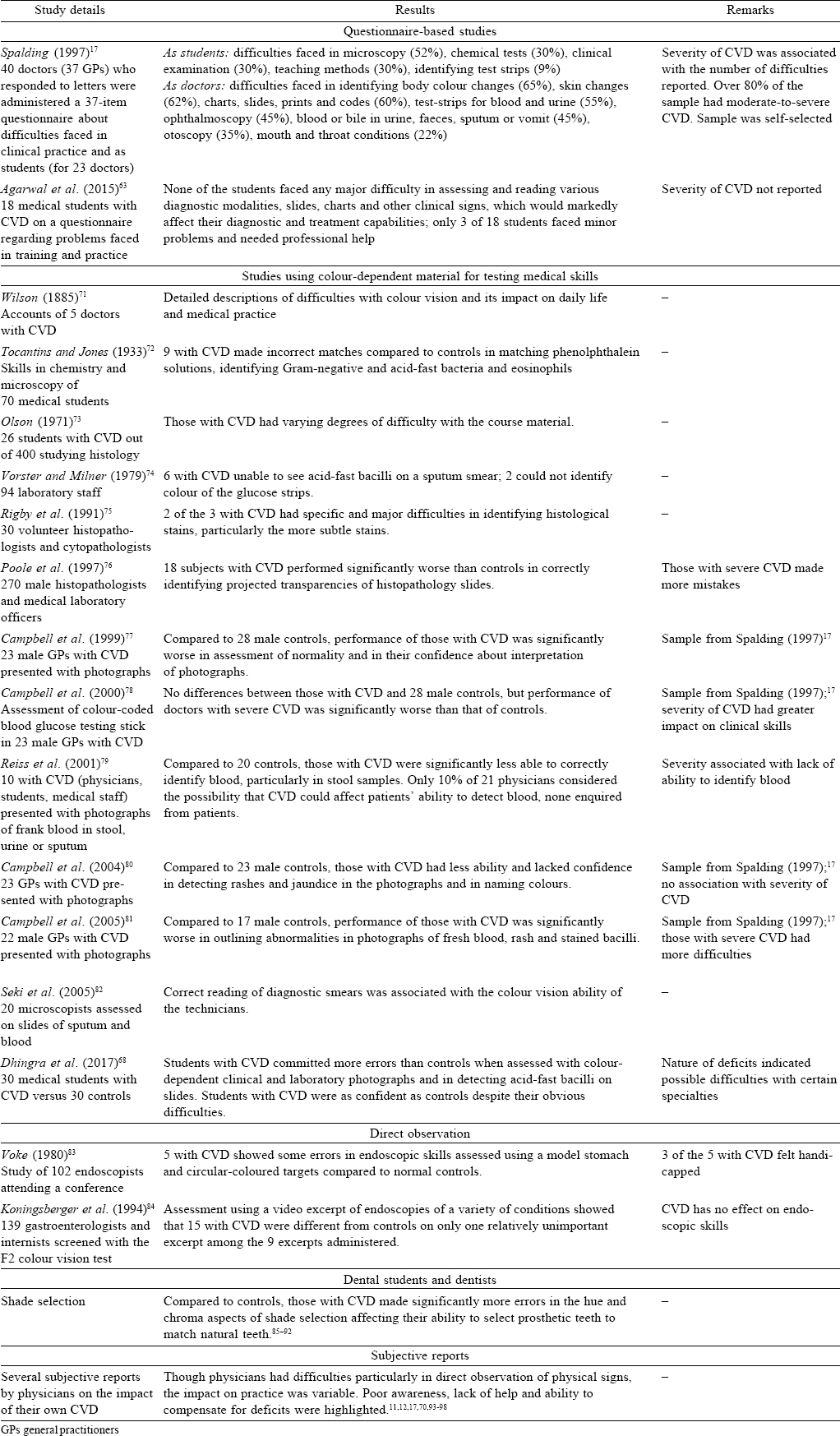
Despite the limited number of studies on the issue, certain conclusions about the difficulties faced by students, doctors and other medical workers with CVD can be drawn. First, there is reasonable evidence that a certain proportion of medical professionals with CVD face considerable difficulty in training and while carrying out their duties. A consistent finding is that the severity of CVD is associated with the level of performance across most of the studies that have examined severity. Accordingly, subjects with mild-to-moderate CVD often do not report facing any difficulties at all. In contrast, those with severe CVD not only experience considerable difficulties in their work but are also at greater risk of committing diagnostic and treatment errors, some of which may have potentially serious consequences. This affects the confidence of persons with CVD and diminishes their performance of medical duties. However, even the evidence for these observations is often variable and inconsistent. Almost all studies have small sample size and in some instances consist of self-selected doctors with mostly severe CVD.[17].[77],[78],[79],[80],[81] Therefore, none of these findings can be considered conclusive unless larger and more representative samples are examined. The relative lack of naturalistic studies in actual clinical conditions creates further problems in interpreting the results of these studies. First test conditions differ from real-world conditions in many ways such as illumination, speed and time pressure or working alone and during home visits, all of which cannot be replicated in test conditions. Second, doctors with significant deficits due to CVD often use other methods such as more intensive observation or examination, cross-checking, greater efforts to obtain information from other sources and seeking help from others colleagues to overcome their difficulties. They also tend to use additional cues from history and examination to compensate for the handicaps resulting from CVD. Finally, clinical decision-making is a complex process and none of these studies provide evidence for a causal relationship between the difficulties reported due to CVD and patient management. Although doctors with CVD might commit errors in recognizing colour-dependent signs or findings, the extent and seriousness of these errors are not clearly evident from the existing studies. Medical errors are not uncommon and can result both from personal reasons as well as flaws in the system. It is likely that most of these errors due to CVD can be prevented by anticipating them and instituting preventative measures. It has been suggested that the risk of committing errors is minimized if circumstances are optimal (e.g. good illumination, use of aids, teamwork), when rapidity and time demands are not involved (e.g. in emergency settings) and where decision-making does not involve a single pivotal colour-dependent observation (e.g. severe bleeding).[11]·[56]·[57]·[70]·[92]
Awareness of CVD
Much like other people, many doctors are unaware of the severity of their CVD and assume their disability to be of little consequence.[17]·[70] Two of the three histopathologists in the study by Rigby et al.[75] were unaware of their deficiency, while Spalding[17] found that 19 of their 24 general practitioners with severe CVD did not know about their problems, while many became aware about the extent of their CVD much later. Similar low levels of awareness have been found among Indian medical students.[65] Lack of awareness could stem from the fact that medical professionals are not screened for CVD or the extent of their CVD is not assessed properly.[17],[83] The overwhelming maj ority of Indian medical students are likely to be screened for CVD only at the time of entry to the MBBS course, accounting for their unawareness.[68] Moreover, those with less severe CVD learn to cope with their handicaps using cues or seeking help from others.[17]·[56]·[57]·[70] Finally, there is an element of denial, which might arise from the stigma associated with CVD and the fear that acknowledgement might hamper their careers.[12]·[13]·[96] Due to these concerns, students and doctors with CVD often project themselves as competent professionals even in the face of obvious difficulties.[17]·[68]·[96]
Choice of specialties
It has been proposed that CVD could pose special difficulties in certain specialties and cause less problems with others. Much of the evidence for this contention derives from the study of Spalding, where 23 doctors were asked about the specialties they would have avoided as students.[17]·[70]·[99] The specialties mentioned were histology, haematology, bacteriology, surgery, pathology, dermatology, anaesthesiology and retinal work in ophthalmology. The second piece of evidence derives from the studies listed in [Table - 4], which suggest that difficulties may be faced in microscopy (52%), chemical tests (30%), clinical examination (30%) and teaching methods (30%). This has been taken as evidence that doctors with CVD should avoid the specialties of histology, pathology, bacteriology, surgery, dermatology, ENT, anaesthe- siology, emergency medicine, general practice, paediatrics, biochemistry and ophthalmology, while psychiatry, neurology and radiology should not pose problems.[11]·[17]·[56],[57],[58]·[68]·[70] However, it is obvious that such lists are not definitive because they are based on insufficient, anecdotal and selective evidence while ignoring the efforts that can be or are made by doctors with CVD working in different specialties.
Rights of medical professionals with CVD and avoiding discrimination
All over the world, there is growing awareness of the need to provide equal opportunities to those who have disabilities.[13]·[38] Although CVD does not strictly qualify as a disability, the need to avoid discriminating against individuals with CVD because of their deficiency is an important issue.[38] Any restriction of rights of those with handicaps can only be allowed if it can be conclusively demonstrated that they cannot meet the requirements of the job even after all help has been provided to mitigate effects of the deficiency, and/or that allowing such persons to work would compromise their safety or the safety of others. Based on the extant literature, it is evident that conclusive evidence linking CVD with occupational difficulties and risks is lacking. Rather, the evidence suggests that with proper awareness most people with CVD will be able to work properly and safely.[42] Consequently, almost all professions that restrict employment of those with CVD are gradually relaxing their requirements for colour vision standards.[13]·[38]·[42] For doctors with CVD, the principle of equal opportunity translates as striking a balance between patient welfare with the necessity of equal and inclusive handling of those with CVD. Since the evidence connecting CVD with difficulties at work in the medical profession is even more scarce and debatable, avoiding unnecessary discrimination is a more pertinent concern.[92],[96] The consensus view is that the presence of CVD should not be used to debar those who seek to become a part of the medical profession. Accordingly, apart from a few exceptions, medical courses all over the world do not exclude students with CVD. Alternatively, early detection, improving awareness, counselling to provide informational, emotional and practical help are not just ethical measures but realistic necessities in the practice of medicine.[11]·[57]·[68]·[70]·[100] Although there is a move away from whole-population screening for CVD, particularly at the school level, pre-vocational screening is still considered a justifiable measure.[13]·[21]·[22]·[42]·[101]·[102] Screening has been repeatedly recommended before entry to MBB S and is especially relevant in the Indian situation because those with CVD are considerably less likely to have been screened at any earlier stage.[68] Although several practical aids which could help doctors with CVD overcome their difficulties have been suggested, the only pragmatic way to help doctors with CVD is to make them aware of the nature and extent of their deficiency and offer constant support throughout their careers.[2]·[68]·[73]·[103] Unfortunately, it appears that the majority of doctors with CVD usually do not receive such help and support.[11]·[17]·[56]·[70]·[104] This shortcoming needs to be addressed by future research and practice in this area.
Conclusion
This overview of CVD shows that research on psychosocial aspects of CVD is rather limited, particularly regarding the impact of CVD on the medical profession. Obviously, much more needs to be done before making definitive statements on this sensitive issue. Nevertheless, the existing evidence, including data from general-population studies, highlights that some people with CVD including doctors may face difficulties in daily life and work. The nature and severity of CVD, awareness of its impact, personal circumstances and the ability to cope with colour vision deficits are the major factors that determine the eventual impact of CVD. Therefore, early detection, enhancing awareness and offering help will mitigate much of the adverse impact of CVD among those intending to or already pursuing a career in medicine. Such measures will also help in striking a balance between patient-related concerns and rights of doctors with CVD to fulfil their career-related ambitions. Thus, despite the scarcity of the evidence, it is possible to formulate a few broad and tentative recommendations given in [Box 1].

Conflicts of interest. None declared
| 1. | Times of India; 31 July 2017. Available at www.timesofindia.indiatimes.com/ india/mci-agrees-to-allow-colour-blind-students-in-medical-colieges/ articleshow/59850459.cms (accessed on 12 Sep 2017). [Google Scholar] |
| 2. | Simunovic MP. Colour vision deficiency. Eye (Lond) 2010;24:747–55. [Google Scholar] |
| 3. | Chan XB, Goh SM, Tan NG. Subjects with colour vision deficiency in the community: What do primary care physicians need to know? Asia Pac Fam Med 2014;13:10. Available at www.apfmj.com/content/13/1/10 (accessed on 15 Sep 2017). [Google Scholar] |
| 4. | Birch J. Worldwide prevalence ofred-green color deficiency. J Opt SocAm A Opt Image Sci Vis 2012;29:313–20. [Google Scholar] |
| 5. | Cole BL. Assessment of inherited colour vision defects in clinical practice. Clin Exp Optom 2007;90:157–75. [Google Scholar] |
| 6. | Moudgil T, Arora R, Kaur K. Prevalence of colour blindness in children. Int J Med Dent Sci 2016;5:1252–8. [Google Scholar] |
| 7. | Chakrabarti A, Chakraborti S. Red-green color vision deficiency and lack of awareness among rural school students in India. Iran J Public Health 2015;44: 1018-20. [Google Scholar] |
| 8. | Kumar R, Kumar J, Soni ND, Choudhary R. Prevalence of colour blindness among school going children aged 10-17 years in Jodhpur city Rajasthan. Sch J Arts Humanit Soc Sci 2016;4:126-9. [Google Scholar] |
| 9. | Shah A, Hussain R, Fareed M, Afzal M. Prevalence of red-green color vision defects among muslim males and females of Manipur, India. Iran J Public Health 2013;42:16-24. [Google Scholar] |
| 10. | Fareed M, Anwar MA, Afzal M. Prevalence and gene frequency of colour vision impairments among children of six populations from North Indian region. Genes Dis 2015;2:211-18. [Google Scholar] |
| 11. | Spalding JA. Colour vision deficiency in the medical profession. Br J Gen Pract 1999;49:469-75. [Google Scholar] |
| 12. | Spalding JA. The doctor with an inherited defect of colour vision: Effect on clinical skills. Br J Gen Pract 1993;43:32-3. [Google Scholar] |
| 13. | Cole BL. The handicap of abnormal colour vision. Clin Exp Optom 2004;87: 258-75. [Google Scholar] |
| 14. | Hurvich LM. Color vision. Sunderland, MA:Sinauer Associates; 1981. [Google Scholar] |
| 15. | Steward JM, Cole BL. What do color vision defectives say about everyday tasks? Optom Vis Sci 1989;66:288-95. [Google Scholar] |
| 16. | Tagarelli A, Piro A, Tagarelli G, Lantieri PB, Risso D, Olivieri RL, et al. Colour blindness in everyday life and car driving. Acta Ophthalmol Scand 2004;82: 436-42. [Google Scholar] |
| 17. | Spalding JA. Doctors with inherited colour vision deficiency: Their difficulties in clinical work. In: Cavonius CR (ed.). Colour Vision DeficienciesXIII. Proceedings of the International Research Group for Colour Vision Deficiency 1995. Vol. 59. Dordrecht:Kluwer Academic Publishers; 1997:483-9. [Google Scholar] |
| 18. | Cole BL. Protan colour vision deficiency and road accidents. Clin Exp Optom 2002;85:246-53. [Google Scholar] |
| 19. | Cole BL. Colour blindness and driving. Clin Exp Optom 2016;99:484-7. [Google Scholar] |
| 20. | Owsley C, McGwin G Jr. Vision and driving. Vision Res 2010;50:2348-61. [Google Scholar] |
| 21. | Ramachandran N, Wilson GA, Wilson N. Is screening for congenital colour vision deficiency in school students worthwhile? A review. Clin Exp Optom 2014; 97:499-506. [Google Scholar] |
| 22. | Cumberland P, Rahi JS, Peckham CS. Impact of congenital colour vision deficiency on education and unintentional injuries: Findings from the 1958 British birth cohort. BMJ 2004;329:1074-5. [Google Scholar] |
| 23. | Vingrys AJ, Cole BL. Are colour vision standards justified for the transport industry? Ophthalmic Physiol Opt 1988;8:257-74. [Google Scholar] |
| 24. | Oladehinde MK, Adeoye AO, Adegbehingbe BO, Onakoya AO. Visual functions of commercial drivers in relation to road accidents in Nigeria. Indian J Occup Environ Med 2007;11:71-5. [Google Scholar] |
| 25. | Isawumi MA, Adeoti CO, Ubah JN, Oluwatimilehin IO, Raj i RA. Ocular status of commercial drivers in Osun state, Nigeria. Afr J Med Med Sci 2011;40:405-11. [Google Scholar] |
| 26. | Biza M, Mossie A, Woldemichael K, Gelaw Y. Visual impairment and road traffic accidents among drivers in Jimma town, Southwest Ethiopia. Ethiop Med J 2013;51:123-32. [Google Scholar] |
| 27. | Shearron GF. Color vision deficiency in primary school children. Sight Sav Rev 1965;35:148-51. [Google Scholar] |
| 28. | Mandola J. The role of color vision anomalies in elementary school achievement. J Sch Health 1969;39:633-6. [Google Scholar] |
| 29. | Lampe JM, Doster ME, Beal BB. Summary of a three-year study of academic and school achievement between color-deficient and normal primary age pupils: Phase two. J Sch Health 1973;43:309-11. [Google Scholar] |
| 30. | Gordon N. Colour blindness. Public Health 1998;112:81^. [Google Scholar] |
| 31. | Wilkinson WK. The cognitive and social-emotional correlates of color deficiency in children: A literature review and analysis. Adolescence 1992;27:603-11. [Google Scholar] |
| 32. | Albany-Ward K, Sobande M. What do you really know about colour blindness? Br J Sch Nurs 2015;10:123-5. [Google Scholar] |
| 33. | Grassivaro Gallo P, Panza M, Viviani F, Lantieri PB. Congenital dyschromatopsia and school achievement. Percept Mot Skills 1998;86:563-9. [Google Scholar] |
| 34. | Grassivaro Gallo P, Oliva S, Lantieri PB, Viviani F. Colour blindness in Italian art high school students. Percept Mot Skills 2002;95:830-4. [Google Scholar] |
| 35. | Suero MI, Perez AL, Diaz F, Montanero M, Pardo PJ, Gil J, et al. Does daltonism influence young children’s learning? Learn Individ Differ 2005;15:89-98. [Google Scholar] |
| 36. | Ugalahi MO, Fasina O, Ogun OA. Impact of congenital color vision defect on color-related tasks among secondary school students in Ibadan, Southwest Nigeria. Niger J Ophthalmol 2016;24:20-4. [Google Scholar] |
| 37. | Grassivaro Gallo P, Panza M, Lantieri PB, Risso D, Conforti G, Lagonia P, et al. Some psychological aspects of colour blindness at school: A field study in Calabria and Basilicata (Southern Italy). Color Res Appl 2003;28:216-20. [Google Scholar] |
| 38. | Birch J, Chisholm CM. Occupational colour vision requirements for police officers. Ophthalmic Physiol Opt 2008;28:524-31. [Google Scholar] |
| 39. | Taylor WO. Effects on employment of defects in colour vision. Br J Ophthalmol 1971;55:753-60. [Google Scholar] |
| 40. | Voke J. Significance of defective colour vision. Rev Prog Coloration 1983;13: 1-9. [Google Scholar] |
| 41. | Cumberland P, Rahi JS, Peckham CS. Impact of congenital colour vision defects on occupation. Arch Dis Child 2005;90:906-8. [Google Scholar] |
| 42. | Rahi JS. Impact of congenital colour vision deficiency. BMJ 2005;330:96. [Google Scholar] |
| 43. | Bailey J. Color Blindness: Psychological Effects; 2013. Available at www.sites. psu. edu/jessikabailey/…/Psychological-Research-Paper_Color-Blindness_ Bailey-J (accessed on 12 Sep 2017). [Google Scholar] |
| 44. | Snyder CR. The psychological implications of being color blind. J Spec Educ 1973;7:51-4. [Google Scholar] |
| 45. | Hertel RK. Analyzing the traumatic impact of childhood visual impairment. J Am Psychoanal Assoc 2003;51:913-39. [Google Scholar] |
| 46. | Lakowski T. Psychological variables in colour vision testing. In: Richter M (ed.). Proceedings of the 1st International Colour Congress, Stockholm, 1969. Volume 1. Gottingen: Muster-Schmidt, Verlag; 1970:79-87. [Google Scholar] |
| 47. | Bradley N. Colour blindness: Notes on its developmental and clinical significance. Int J Psychoanal 1970;51:59-70. [Google Scholar] |
| 48. | Pickford RW, Cobb SR. Personality and colour vision deficiencies. Mod Probl Ophthalmol 1974;13:225-30. [Google Scholar] |
| 49. | Cobb SR. Evidence for an effect by colour defect on personality. Percept Mot Skills 1980;51:159-66. [Google Scholar] |
| 50. | Benjamin J, Press J, Maoz B, Belmaker RH. Linkage of a normal personality trait to the color-blindness gene: Preliminary evidence. Biol Psychiatry 1993;34: 581-3. [Google Scholar] |
| 51. | Perez-Carpinell J, Ibaez Vallejo MC, Diaz Esteve JV. Psychological factors and defective colour vision. In: Drum et al. (eds). Colour Vision Deficiencies XII.Documenta Ophthalmologica Proceedings Series. Vol. 57. Dordrecht:Kluwer Academic Publishers; 1995:221-6. [Google Scholar] |
| 52. | Coren S, Harland RE. Personality correlates of variations in visual and auditory abilities. Pers Individ Dif 1995;18:15-25. [Google Scholar] |
| 53. | Larsson EE, von Stumm S. Seeing red? The effect of colour on intelligence test performance. Intelligence 2015;48:133-6. [Google Scholar] |
| 54. | Maule L, Featonby D. Colour vision deficiency and physics teaching. PhysEduc 2016;51:035005. Available at www.iopscience.org/ped (accessed on 15 Sep 2017). [Google Scholar] |
| 55. | Tagarelli A, Piro A, Tagarelli G. Genetic, epidemiologic and social features of colour blindness. Community Genet 1999;2:30-5. [Google Scholar] |
| 56. | Ali L. Color vision deficiency (CVD) in the medical and allied occupations. JUMDC 2012;3:1-5. [Google Scholar] |
| 57. | Goh SS, Chan VX, Tan NG. Colour vision deficiency: Is it a handicap? A narrative review of its impact on medical and dental education and practice. Proc Sing Healthc 2014;23:149-57. [Google Scholar] |
| 58. | Balasundaram R, Reddy SC. Prevalence of colour vision deficiency among medical students and health personnel. Malays Fam Physician 2006;1:52-3. [Google Scholar] |
| 59. | Pramanik T, Sherpa MT, Shrestha R. Color vison deficiency among medical students: An unnoticed problem. Nepal Med Coll J 2010;12:81-3. [Google Scholar] |
| 60. | Siddiqui QA, Shaikh SA, Qureshi TZ, Subhan MM. A comparison of red-green color vision deficiency between medical and non-medical students in Pakistan. Saudi Med J 2010;31:895-9. [Google Scholar] |
| 61. | Pramanik T, Khatiwada B, Pandit R. Color vision deficiency among a group of students of health sciences. Nepal Med Coll J 2012;14:334-6. [Google Scholar] |
| 62. | Mughal IA, Ali L, Aziz N, Mehmood K, Afzal N. Colour vision deficiency (CVD) in medical students. Pak J Physiol 2013;9:14-16. [Google Scholar] |
| 63. | Agarwal R, Singh P, Nema P, Kumar R, Raghuwanshi S, Gupta SB. Prevalence of colour vision deficiency (CVD) in students of medical college and to assess whether colour blind medical students face any problem in their medical training and profession. J Res Ophthalmol Vis Sci 2015;1:12-15. [Google Scholar] |
| 64. | Patel JR, Trivedi H, Patel A, Patil S, Jethva J. Assessment of colour vision deficiency in medical students. Int J Community Med Public Health 2016;3: 230-5. [Google Scholar] |
| 65. | Subha L, Ramyaa M, Rajarathinam MS. Prevalence of congenital color blindness among under graduate medical students. Int J Pharm Biol Sci 2015;6:1114-16. [Google Scholar] |
| 66. | Saha D, Saha K. Prevalence of colour vision deficiency (CVD) in medical students in Kolkata, West Bengal. IOSR J Dent Med Sci 2016;15:1-3. [Google Scholar] |
| 67. | Lashari MK, Mahmood B, Razzaq A. Prevalence of color vision deficiency among the students of Quaid-e-Azam Medical College, Bahwalpur, Punjab, Pakistan. Int J Res 2016;3:1199-204. [Google Scholar] |
| 68. | Dhingra R, Rohatgi J, Dhaliwal U. Preparing medical students with congenital colour vision deficiency for safe practice. Natl Med J India 2017;30:30-5. [Google Scholar] |
| 69. | Khalid M, Chughtai MA, Mian HI, Shah SN. Frequency of colour vision deficiency among dental students. Pak Oral Dent J 2017;37:161-3. [Google Scholar] |
| 70. | Spalding JA. Medical students and congenital colour vision deficiency: Unnoticed problems and the case for screening. Occup Med (Lond) 1999;49:247-52. [Google Scholar] |
| 71. | Wilson G. Researches on colour-blindness: With a supplement on the danger attending the present system of railway and marine coloured signals. Edinburgh:Sutherland and Knox; 1855. [Google Scholar] |
| 72. | Tocantins LM, Jones JW. Defective colour vision and its handicaps in medicine. Am J Sci 1993;293:243–9. [Google Scholar] |
| 73. | Olson IA. The use of colour filters by students with congenital colour defects in the learning of histology. Med Biol Illus 1971;21:52-3. [Google Scholar] |
| 74. | Vorster BJ, Milner LV. Colour-blind laboratory technologists. Lancet 1979;2:1295. [Google Scholar] |
| 75. | Rigby HS, Warren BF, Diamond J, Carter C, Bradfield JW. Colour perception in pathologists: The Farnsworth-Munsell 100-hue test. J Clin Pathol 1991 ;44: 745-8. [Google Scholar] |
| 76. | Poole CJ, Hill DJ, Christie JL, Birch J. Deficient colour vision and interpretation of histopathology slides: Cross sectional study. BMJ 1997;315:1279-81. [Google Scholar] |
| 77. | Campbell JL, Spalding AJ, Mir FA, Birch J. Doctors and the assessment of clinical photographs—Does colour blindness matter? Br J Gen Pract 1999;49:459-61. [Google Scholar] |
| 78. | Campbell JL, Spalding JA, Mir FA, Birch J. Doctors and the assessment of blood glucose testing sticks: Does colour blindness matter? Br J Gen Pract 2000;50: 393-5. [Google Scholar] |
| 79. | Reiss MJ, Labowitz DA, Forman S, Wormser GP. Impact of color blindness on recognition of blood in body fluids. Arch Intern Med 2001;161:461-5. [Google Scholar] |
| 80. | Campbell JL, Spalding JA, Mir FA. The description of physical signs of illness in photographs by physicians with abnormal colour vision. Clin Exp Optom 2004; 87:334-8. [Google Scholar] |
| 81. | Campbell JL, Griffin L, Spalding JA, Mir FA. The effect of abnormal colour vision on the ability to identify and outline coloured clinical signs and to count stained bacilli in sputum. Clin Exp Optom 2005;88:376-81. [Google Scholar] |
| 82. | Seki N, Yassin MA, Cuevas LE, Wendy Bailey J, Bertel Squire S, Ramsay A, et al. Short communication: Colour vision and proficiency in diagnostic microscopy. Trop Med Int Health 2005;10:433–4. [Google Scholar] |
| 83. | Voke JE. Colour vision testing in specific industries and professions. London:Keeler; 1980. [Google Scholar] |
| 84. | Koningsberger JC, van Norren D, van Niel JC, Dekker W. Does color vision deficiency in the endoscopist influence the accuracy of endoscopic diagnosis? An anonymous study with Dutch gastrointestinal endoscopists. Endoscopy 1994;26:549–53. [Google Scholar] |
| 85. | Barna GJ, Taylor JW, King GE, Pelleu GB Jr. The influence of selected light intensities on color perception within the color range of natural teeth. J Prosthet Dent 1981;46:450–3. [Google Scholar] |
| 86. | Davison SP, Myslinski NR. Shade selection by color vision-defective dental personnel. J Prosthet Dent 1990;63:97-101. [Google Scholar] |
| 87. | Curd FM, Jasinevicius TR, Graves A, Cox V, Sadan A. Comparison of the shade matching ability of dental students using two light sources. J Prosthet Dent 2006;96:391-6. [Google Scholar] |
| 88. | Ethell J, Jarad FD, Youngson CC. The effect of colour defective vision on shade matching accuracy. Eur J Prosthodont Restor Dent 2006;14:131-6. [Google Scholar] |
| 89. | Gokce HS, Piskin B, Ceyhan D, Gokce SM, Arisan V. Shade matching performance of normal and color vision-deficient dental professionals with standard daylight and tungsten illuminants. J Prosthet Dent 2010;103:139–47. [Google Scholar] |
| 90. | Borbély J, Varsányi B, Fejérdy P, Hermann P, Jakstat HA. Toothguide trainer tests with color vision deficiency simulation monitor. J Dent 2010;38 Suppl 2:e41-9. [Google Scholar] |
| 91. | Vafaee F, Rakhshan V, Vafaei M, Khoshhal M. Accuracy of shade matching performed by colour blind and normal dental students using 3D master and Vita Lumin shade guides. Eur J Prosthodont Restor Dent 2012;20:23–5. [Google Scholar] |
| 92. | Mushtaq F, Baraas RC, Al-Saud LM, Mirghani I, van der Zee C, Yates E, et al. Should prospective dental students be screened for colour vision deficits? Br Dent J 2016;221:227-8. [Google Scholar] |
| 93. | Logan JS. The disability in so-called red-green blindness: An account based on many years of self-observation. Ulster Med J 1977;46:41-5. [Google Scholar] |
| 94. | Currier JD. A two and a half colour rainbow. Arch Neurol 1994;51:1090-2. [Google Scholar] |
| 95. | Goudie RB. Colour deficient vision should not prevent a career in histopathology. BMJ 1998;316:1750. [Google Scholar] |
| 96. | Spalding JA. Confessions of a colour blind physician. Clin Exp Optom 2004;87: 344-9. [Google Scholar] |
| 97. | Cockburn DM. Confessions of a colour blind optometrist. Clin Exp Optom 2004;87:350-2. [Google Scholar] |
| 98. | Wiegersma PA. Impact of CVD on medical practice. BMJ 2004;329:1074. [Google Scholar] |
| 99. | Spalding JA. Doctors with daltonism and the implications for counselling. Optom Today 2002;42:23-5. [Google Scholar] |
| 100. | Spalding JA, Cole BL, Mir FA. Advice for medical students and practitioners with colour vision deficiency: A website resource. Clin Exp Optom 2010;93:39-41. [Google Scholar] |
| 101. | Cole BL. Impact of congenital colour vision deficiency: Congenital colour vision deficiency does cause problems. BMJ 2005;330:96. [Google Scholar] |
| 102. | Cole BL. Is screening for congenital colour vision deficiency in school students worthwhile? Clin Exp Optom 2015;98:193. [Google Scholar] |
| 103. | Rubin LR, Lackey WL, Kennedy FA, Stephenson RB. Using color and grayscale images to teach histology to color-deficient medical students. Anat Sci Educ 2009;2:84-8. [Google Scholar] |
| 104. | Burke E. Verbatim responses of 155 medical students with colour vision deficiency. Available at www.colourmed.com/I6%20Burca%20 Report.pdf (accessed on 15 Sep 2017). [Google Scholar] |
Fulltext Views
4,019
PDF downloads
1,437




