Translate this page into:
Systemic thrombosis due to pulmonary tuberculosis
Corresponding Author:
Jyotsna M Joshi
Department of Pulmonary Medicine, Topiwala National Medical College and B.Y.L. Nair Hospital, Mumbai 400008, Maharashtra
India
drjoshijm@gmail.com
| How to cite this article: Bansal S, Utpat K, Joshi JM. Systemic thrombosis due to pulmonary tuberculosis. Natl Med J India 2017;30:201-202 |
Abstract
Pulmonary tuberculosis (TB) is an established cause of venous thrombosis. A few instances have been described with arterial thrombosis as well. It has been speculated that TB causes systemic hypercoagulability, which may lead to venous thrombosis. This may be the presenting phenomenon, may occur shortly after diagnosis of TB, or even after starting antitubercular therapy. We describe a patient of pulmonary TB, who presented with pulmonary thromboembolism, with both arterial as well as venous thrombosis, which resolved on antitubercular therapy.
Introduction
Venous thromboembolism encompasses a spectrum of manifestations from deep vein thrombosis (DVT) to pulmonary thromboembolism. Tuberculosis (TB) is a risk factor for the development of venous thromboembolism irrespective of the presence of other contributing factors. However, the association of arterial thrombosis with TB is rare.[1],[2] We report a 31-year-old man who presented with systemic thrombosis and pulmonary arterial and venous thromboembolism attributable to pulmonary TB.
The Case
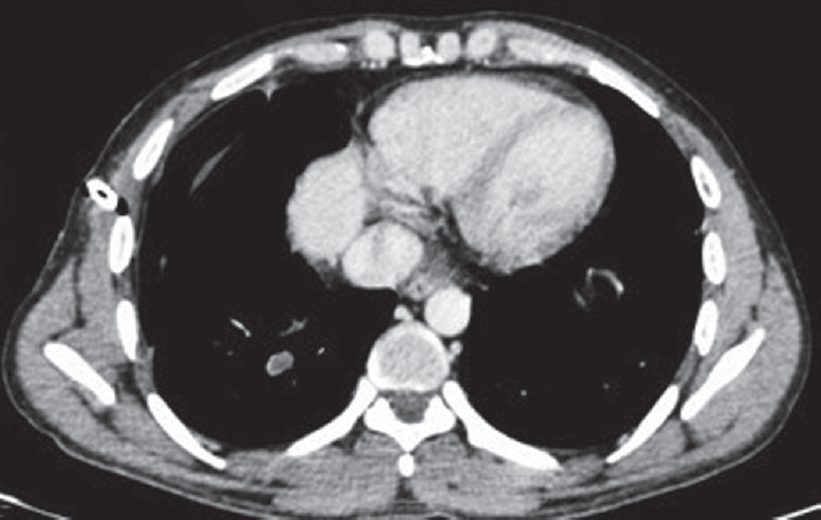
A 31 -year-old man, driver by occupation, presented with 15 days’ history of dyspnoea, cough with mucoid expectoration and fever. There was no history of chest pain or haemoptysis. He was initially evaluated by a physician with a chest X-ray, which showed a small right-sided small pleural effusion. The patient was managed with empirical antibiotic therapy. However, in view of increased dyspnoea over 2 days he came to our clinic. At presentation his pulse rate was 112/minute, blood pressure of 110/ 70 mmHg and respiratory rate of 32 cycles/minute. Haemoglobin level was 14.3 g/dl, white cell count of 26 000/cmm and platelet count of 300 000/cmm. HIV was non-reactive, and past or family history was unremarkable. Chest X-ray at admission showed right-sided hydropneumothorax with a patchy consolidation in the right mid-zone, with shift of the mediastinum to the opposite side. A 14-French pigtail catheter was inserted and patient was relieved of his dyspnoea. CT thorax showed right-sided hydropneumothorax, with patchy consolidation in the right upper lobe, consolidation with cavitation in the right lower lobe, and a complete filling defect of the right main pulmonary artery. He was started on anticoagulants, with low molecular weight heparin and warfarin. CT pulmonary angiography showed a thrombus in the right pulmonary artery [Figure - 1] and the right inferior pulmonary vein [Figure - 2] with a large splenic infarct. Sputum Gene Xpert done at our laboratory was reported as ‘MTB detected, rifampicin- sensitive’. Two sputum smear samples were negative; however, subsequent TB MGIT culture isolated MTB complex. He was initiated on first-line antitubercular drugs based on the gene Xpert report (isoniazid 75 mg, rifampicin 150 mg, ethambutol 275 mg and pyrazinamide 400 mg). His bilateral lower limb Doppler was normal; 2D-echocardiography showed mild pulmonary hypertension with pulmonary artery systemic pressure as estimated by tricuspid regurgitation jet of 40 mmHg, without any evidence of right ventricular dysfunction. CT abdominal angiography to evaluate the splenic infarct showed complete thrombosis of the splenic vein [Figure - 3] and partial occlusion of the common hepatic artery and gastroduodenal artery. In view of multiple arterial and venous thrombosis, the possibility of inherited thrombophilia was considered, and the patient was evaluated with a complete thrombophilia profile consisting of protein C, protein S, antithrombin III, antiphospholipid antibody (APLA), factor V leiden mutation, methylene tetrahydrofolate reductase (MTHFR) mutation, homocysteine levels, and activated protein C resistance. All were within normal limits. The patient’s symptoms started improving while on antitubercular therapy. The pigtail catheter was removed after complete expansion of the lung and the patient was discharged on antitubercular therapy and warfarin. At 6 months of follow-up, chest X-ray showed resolution of the right upper lobe consolidation, sputum AFB MGIT culture was negative and the patient was asymptomatic.
 |
| Figure 1: Right main pulmonary artery thrombus |
 |
| Figure 2: Right inferior pulmonary vein thrombus |
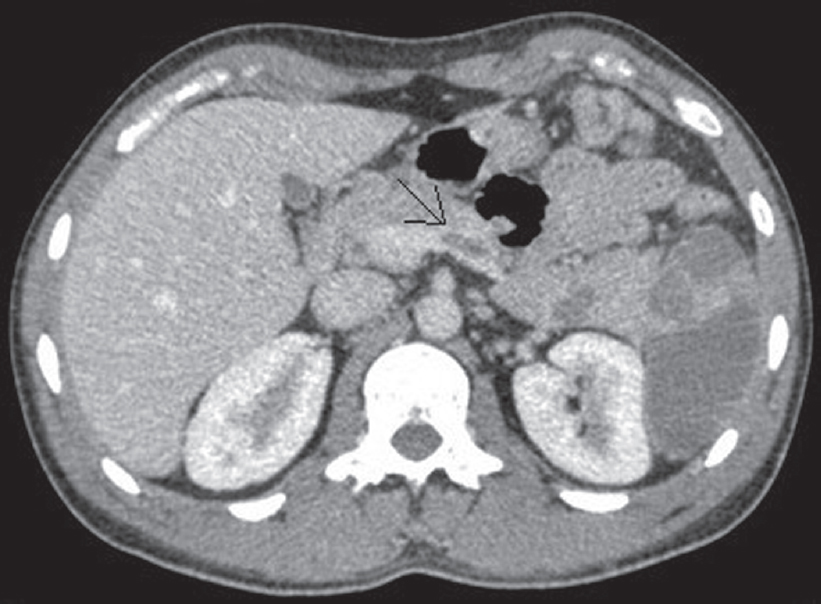 |
| Figure 3: Splenic vein thrombosis |
Discussion
TB is a common infectious disease in India with high morbidity. It can have myriad presentations. Thromboembolic phenomena could occur as the presenting manifestation, complication or sequelae during the course of the disease.[3] Our patient had pulmonary thromboembolism as a rare presenting feature of the disease. Thromboembolism may occur a few days after the diagnosis[4] or late in the course of the disease, even in patients on antitubercular treatment. In the 1980s, White et al. mentoned that the rate of DVT was 3.4% within two weeks after initiation of therapy.[5] In 2006, an Italian study group concluded that the prevalence of venous thromboembolism was 0.6% in the first month of treatment, one-third occurring in the first week.[6]
It has been established that TB is an independent risk factor for venous thrombosis. In the MEDENOX study, patients with TB were found to have a greater risk of venous thromboembolism, close to neoplasia with an odds ratio of 1.62.[7] Widespread TB leading to a transitory hypercoagulable state due to widespread inflammation has also been documented.[8][9] Turken et al. showed that patients with active pulmonary TB had thrombocytosis and increased fibrinogen, factor VIII, and plasminogen activator inhibitor 1 plasma levels, associated with depressed antithrombin III and protein C levels in the first month of treatment, resulting in activated coagulation and inhibited fibrinolysis.
Experimental studies have also shown the role of proinflammatory cytokines (interleukin 1, interleukin 6, tumour necrosis factor α) produced during the acute phase of TB, either by peripheral blood mononuclear cells, or by lung, lymph node and spleen macrophages, and their interaction with mycobacterial products.[10][11] It has also been shown that, in vitro, M. tuberculosis induces the expression of a tissue factor in monocytes–macrophages, that is, a primary activator of the clotting cascade.[12] Some authors have postulated that various local factors may also lead to thrombosis such as from venous compression by lymph nodes, as retroperitoneal adenopathies may cause inferior vena cava thrombosis in the absence of any haemostatic abnormalities.[3] However, Dentan et al. felt that systemic rather than local factors play a predominant role.[13] Our patient also indicates the same. Our patient responded well upon initiation of antitubercular therapy, and continues to be symptom-free. This is in concordance with a few studies suggesting that patients with haemodynamic instability improved with antitubercular treatment within 4 weeks.[8]
There have been many case reports of TB associated with upper and lower limb DVT, hepatic vein,[14] retinal vein[15] and cerebral venous sinus thrombosis.[16] However, only a few have reported TB associated with arterial thrombosis.[1][2][17] We report this patient as it shows a rare presentation of TB with both arterial and venous thrombosis. It is a potentially treatable condition if diagnosed and managed early.
| 1. | Sharma A, Sharma V. Abdominal aortic thrombosis and tuberculosis: An uncommon association. Gastroenterol Rep (Oxf) 2014;2:311-12. [Google Scholar] |
| 2. | Nicholson G, Sachdev AK. Axillary artery occlusion and pulmonary tuberculosis. BMJ 1976;4:626 [Google Scholar] |
| 3. | Gogna A, Pradhan GR, Sinha RS, Gupta B. Tuberculosis presenting as deep vein thrombosis. Postgrad Med J 1999;75:104-5. [Google Scholar] |
| 4. | Sharma RR, Acharya KV, Poornima V. A rare complication of pulmonary tuberculosis—Case report. J Indian Assoc Clin Med 2007;8:179-81. [Google Scholar] |
| 5. | White NW. Venous thrombosis and rifampicin. Lancet 1989;2:434-5. [Google Scholar] |
| 6. | Ambrosetti M, Ferrarese M, Codecasa LR, Besozzi G, Sarassi A, Viggiani P, et al.; AIPO/SMIRA TB Study Group. Incidence ofvenous thromboembolism in tuberculosis patients. Respiration 2006;73:396. [Google Scholar] |
| 7. | Alikhan R, Cohen AT, Combe S, Samama MM, Desjardins L, Eldor A, et al.; MEDENOX Study. Risk factors for venous thromboembolism in hospitalized patients with acute medical illness : Analysis of the MEDENOX Study. Arch Intern Med 2004;164:963-8. [Google Scholar] |
| 8. | Turken O, Kunter E, Sezer M, Solmazgul E, Cerrahoglu K, Bozkanat E, et al. Hemostatic changes in active pulmonary tuberculosis. Int J Tuberc Lung Dis 2002;6:927-32. [Google Scholar] |
| 9. | Robson SC, White NW, Aronson I, Woollgar R, Goodman H, Jacobs P. Acute-phase response and the hypercoagulable state in pulmonary tuberculosis. Br J Haematol 1996;93:943-9. [Google Scholar] |
| 10. | Hussain R, Shiratsuchi H, Phillips M, Ellner J, Wallis RS. Opsonizing antibodies (IgG1) up-regulate monocyte proinflammatory cytokines tumour necrosis factoralpha (TNF-alpha) and IL-6 but not anti-inflammatory cytokine IL-10 in mycobacterial antigen-stimulated monocytes-implications for pathogenesis. Clin Exp Immunol 2001;123:210-18. [Google Scholar] |
| 11. | Valone SE, Rich EA, Wallis RS, Ellner JJ. Expression of tumor necrosis factor in vitro by human mononuclear phagocytes stimulated with whole Mycobacterium bovis BCG and mycobacterial antigens. Infect Immun 1988;56:3313-15. [Google Scholar] |
| 12. | Kothari H, Rao LV, Vankayalapati R, Pendurthi UR. Mycobacterium tuberculosis infection and tissue factor expression in macrophages. PLoS One 2012;7:e45700. doi: 10.1371/journal.pone.0045700. [Google Scholar] |
| 13. | Dentan C, Epaulard O, Seynaeve D, Genty C, Bosson JL. Active tuberculosis and venous thromboembolism: Association according to international classification of diseases, ninth revision hospital discharge diagnosis codes. Clin Infect Dis 2014;58:495-501. [Google Scholar] |
| 14. | Gogna A, Grover S, Arun A, Saluja S. Isolated hepatic inferior vena cava thrombosis in a case of tuberculosis—Case report. J Indian Assoc Clin Med 2004;5:266-8. [Google Scholar] |
| 15. | Fullerton DG, Shrivastava A, Munavvar M, Jain S, Howells J, Macdowall P. Pulmonary tuberculosis presenting with central retinal vein occlusion. Br J Ophthalmol 2007;91:1714-15. [Google Scholar] |
| 16. | Fiorot Júnior JA, Felício AC, Fukujima MM, Rodrigues CA, Morelli VM, Lourenço DM, et al. Tuberculosis: An uncommon cause of cerebral venous thrombosis? Arq Neuropsiquiatr 2005;63 (3B):852-4. [Google Scholar] |
| 17. | Vaideeswar P, Deshpande JR. Non-atherosclerotic aorto-arterial thrombosis: A study of 30 cases at autopsy. J Postgrad Med 2001;47:8-14. [Google Scholar] |
Fulltext Views
2,075
PDF downloads
535




